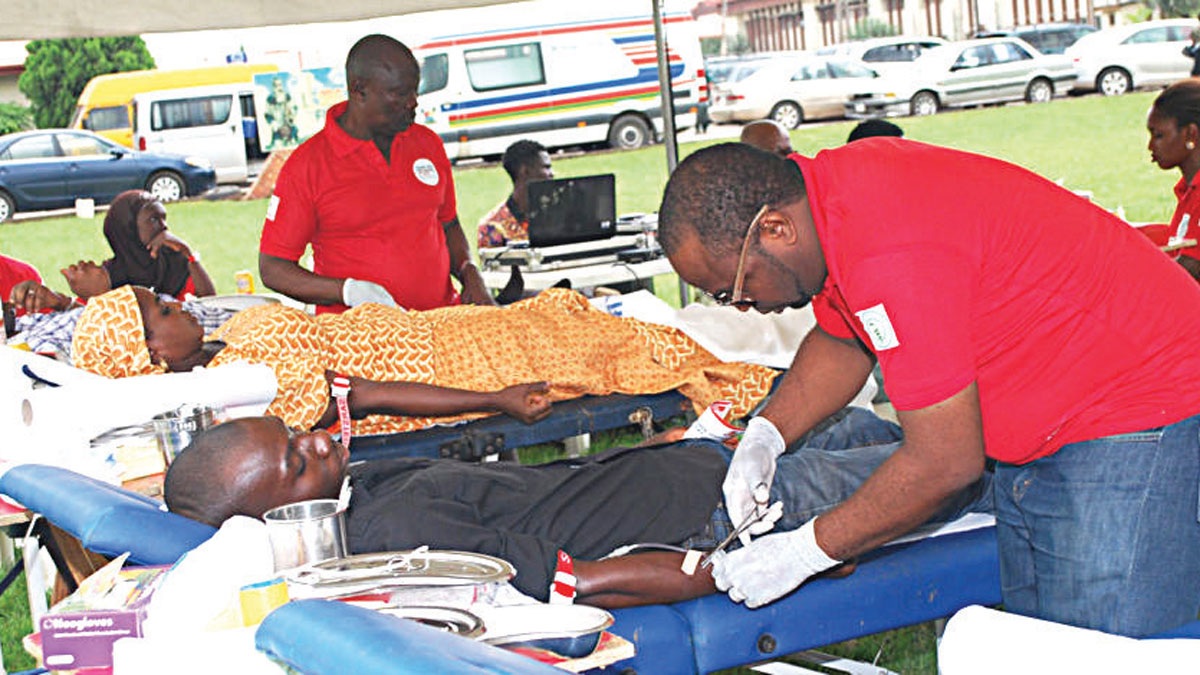
Today is World Blood Donor Day (WBDD). Despite efforts over the years to raise awareness on safe blood and encourage voluntary donation, poor donor and transfusion practices persist in Nigeria.
Several studies have shown that blood transfusion services are essential components of the healthcare delivery system. Unfortunately, in Sub-Saharan Africa most secondary and tertiary hospitals run inadequate and inefficient blood bank services.
Most countries in Sub- Saharan Africa have national blood policies but blood transfusion services remain inadequate and inefficient. In Nigeria, the National Blood policy recommends obtaining blood from regular, voluntary, non-remunerated donors, screening for Human Immuno-deficiency Virus (HIV)/Acquired Immune Deficiency Syndrome (AIDS), Hepatitis B, Hepatitis C and syphilis. It also requires that records be kept in a uniform and specified manner while maintaining confidentiality.
There are three types of blood donors: voluntary unpaid; family/replacement; and paid.However, report from the Federal Ministry of Health (FMoH), indicates that in most cases, the demand for blood far outweighs the supply. In Nigeria, about 500,000 units of blood are collected yearly out of the required 1.5 million units of blood.
The Guardian investigation revealed that blood is usually obtained on an emergency basis. The typical scenario is that of a patient with an urgent need of a blood transfusion, and the doctor asks the patient’s relatives to provide blood. The relatives donate blood or procure blood from private laboratories and blood banks.They may also enlist the services of commercial blood donors, popularly known as “blood touts”.
Indeed, a poor blood donation culture exists in sub-Saharan Africa and several studies have shown that this is fuelled by religious, spiritual and superstitious beliefs. A study on blood donor practices at two blood banks in Bayelsa State, published in Journal of Medicine and Medical Sciences, observed a defective recording system, that records only potential donors whose haemoglobin levels were above the cut off mark of 12g/dl.
According to the researchers from Faculty of Basic Medical Sciences, College of Health Sciences, Niger Delta University, Amassoma, Wilberforce Island, Bayelsa State, donor demographics were also not well recorded. Donors’ ages ranged from 15 years to 60 years, with 98 per cent of them being male.
Also, 80.6 per cent of donors were commercial/professional donors, with only 0.93 per cent being voluntary donors. 2.89 per cent of potential donors were positive for markers of transmissible infections and were deferred. 80 per cent of the deferred donors were positive for HBsAg, while 14.28 per cent were positive for HIV. The blood group O Rh D positive was the commonest blood group.
HBsAg (also known as the Australia antigen) is the surface antigen of the hepatitis B virus (HBV). It indicates current hepatitis B infection.The researchers concluded: “A poor recording/documentation system is used in the screening of potential blood donors in the blood banks examined. The donor screening system needs to be overhauled. Deferred donors also need to be counselled. A poor blood donation culture exists which needs urgent but definite strategies to overcome.”
According to the World Health Organisation (WHO), blood is an important resource, both for planned treatments and urgent interventions. It can help patients suffering from life-threatening conditions live longer and with a higher quality of life, and supports complex medical and surgical procedures. Blood is also vital for treating the wounded during emergencies of all kinds (natural disasters, accidents, armed conflicts) and has an essential, life-saving role in maternal and perinatal care.
A blood service that gives patients access to safe blood and blood products in sufficient quantity is a key component of an effective health system. Ensuring safe and sufficient blood supplies requires the development of a nationally coordinated blood transfusion service based on voluntary non-remunerated blood donations. However, in many countries, blood services face the challenge of making sufficient blood available, while also ensuring its quality and safety.
The lives and health of millions of people are affected by emergencies every year. In the last decade, disasters have caused more than one million deaths, with more than 250 million people being affected by emergencies every year. Natural disasters such as earthquakes, floods and storms create considerable needs for emergency health care, while at the same time, often destroying vital health facilities as well. Man-made disasters such as road accidents and armed conflicts also generate substantial health care demands and the need for front-line treatment.
Blood transfusion is an essential component of emergency health care. Emergencies increase the demand for blood transfusion and make its delivery challenging and complex. Adequate supply of blood during emergencies requires a well-organized blood service, and engaging the entire community and a blood donor population committed to voluntary unpaid blood donation throughout the year can only ensure this.
This year’s WBDD campaign focuses on blood donation in emergencies. In crisis or emergency situation, the natural human response is “What can I do? How can I help?” Therefore, the slogan for the 2017 campaign is: What can you do? with the secondary message: Give blood. Give now. Give often.
The host country for the global event of World Blood Donor Day 2017 is Viet Nam through its National Institute of Haematology and Blood Transfusion (NIHBT). The Global event will be held in Hanoi today, June 14 2017.
The campaign underlines the role every single person can play in helping others in emergency situations, by giving the valuable gift of blood. It also focuses on the fact that it is important to give blood regularly, so that the blood stock is sufficient before an emergency arises.
According to the WHO, the objectives of this year’s campaign are: to encourage all people to strengthen the emergency preparedness of health services in their community by donating blood; to engage authorities in the establishment of effective national blood donor programmes with the capacity to respond promptly to the increase in blood demand during emergencies; to promote the inclusion of blood transfusion services in national emergency preparedness and response activities; to build wider public awareness of the need for committed, year-round blood donation, in order to maintain adequate supplies and achieve a national self-sufficiency of blood; to celebrate and thank individuals who donate blood regularly and to encourage young people to become new donors as well; and to promote international collaboration and to ensure worldwide dissemination of and consensus on the principles of voluntary non-remunerated donation, while increasing blood safety and availability.
According to the WHO, a stable base of regular, voluntary donation, can assure unpaid blood donors an adequate and reliable supply of safe blood. These donors are also the safest group of donors as the prevalence of bloodborne infections is lowest among this group.
World Health Assembly resolution WHA63.12 urges all Member States to develop national blood systems based on voluntary unpaid donations and to work towards the goal of self-sufficiency.Indeed, the risk of transmission of serious infections, including HIV and hepatitis, through unsafe blood and chronic blood shortages brought global attention to the importance of blood safety and availability.
Through its Blood and Transfusion Safety programme, WHO supports countries in developing national blood systems to ensure timely access to safe and sufficient supplies of blood and blood products and good transfusion practices to meet the patients’ need. The programme provides policy guidance and technical assistance to countries for ensuring universal access to safe blood and blood products and work towards self-sufficiency in safe blood and blood products based on voluntary unpaid blood donation to achieve universal health coverage.
To address the issues of poor blood donor and transfusion practices in Nigeria, the Niger Delta University researchers recommend: “Education of the public plays an important role in blood donation. Lack of public awareness was responsible for a high rate of donor deferrals in Trinidad and Tobago, and gaps in knowledge and practice were shown to affect voluntary blood donation in Nigeria.
“There are no deferral registers and deferred donors are not counselled. We suggest the offering of counselling services to deferred donors. We also advocate a comprehensive recording system in our blood banks to enhance referencing and research.”
 Follow Us on Google News
Follow Us on Google News
 Follow Us on Google Discover
Follow Us on Google Discover
