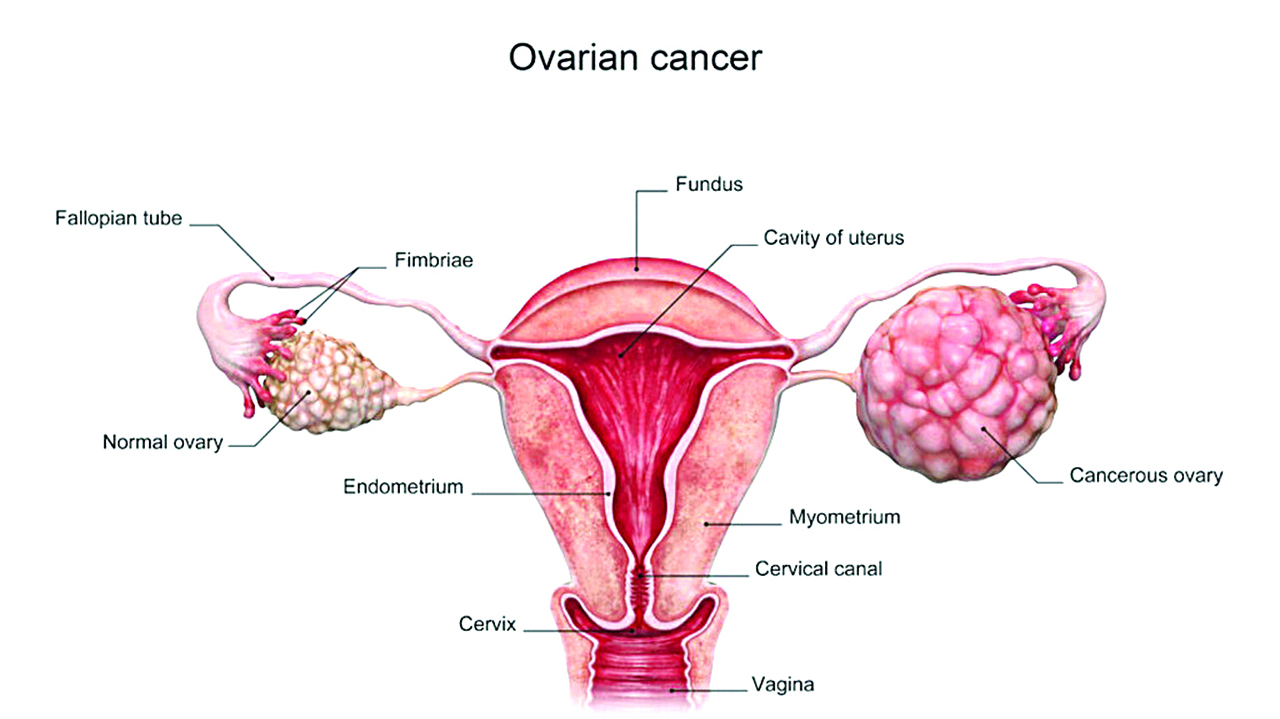
What should people know about ovarian cancer?
OVARIAN cancer is a type of cancer that begins in the ovaries. There are two ovaries in the female reproductive system, with one on each side of the uterus. Each ovary is normally about the size of an almond and they are responsible for producing eggs (ova), as well as hormones, such as estrogen and progesterone. In general, cancer begins when a cell develops errors (mutations) in its DNA. The mutations tell the cell to grow and multiply quickly, creating a mass (tumour) of abnormal cells. The abnormal cells continue living when healthy cells would die. They can invade nearby tissues and break off from an initial tumour to spread to other parts of the body.
What are the warning signs?
Early-stage ovarian cancer rarely causes any symptoms. Advanced-stage ovarian cancer may cause few and non-specific symptoms that are often mistaken for more common benign conditions. Due to these non-specific symptoms or signs, ovarian cancer often goes undetected, until it has spread within the pelvis and abdomen. It is more likely to be treated successfully at the early stage when the disease is confined only to the ovary.
Some of the signs that one may look out for include abdominal bloating or swelling, quickly feeling full when eating, weight loss, feeling of discomfort in the pelvic area, changes in bowel habits particularly constipation, and frequent need to urinate. Women with any of these symptoms and signs should immediately see a doctor, who will commence investigations and then consider if it is necessary to refer to a gynecologist or gynecological oncologist.
Who gets ovarian cancer?
Only women have ovaries; therefore, ovarian cancer can only be found in women. Any female of any age can get ovarian cancer, but it is commoner in those beyond the age of 50 years. It is, however, not clear what causes ovarian cancer, although factors that increase the risk of the disease have been identified.
What are the risk factors?
Factors that can increase a woman’s risk of having ovarian cancer include:
Hereditary: these are inherited gene mutations such as breast cancer gene (BRCA) and with Lynch syndrome. About 10 per cent of ovarian cancers are caused by gene mutations that can be inherited from one’s parents. The breast cancer gene 1 (BRCA1) and breast cancer gene 2 (BRCA2) also increase the risk of breast cancer.
Family history of ovarian cancer: people with two or more close relatives with ovarian cancer have an increased risk of having the disease.
Age: ovarian cancer can occur at any age, but is most common in women aged 50 to 60.
Beginning menstruation at an early age or starting menopause at a later age, or both may also increase the risk of ovarian cancer.
How is ovarian cancer treated?
Ovarian cancer should preferably be treated by a trained gynecological oncologist in a teaching hospital or a comprehensive cancer centre. Surgery and chemotherapy are generally used to treat ovarian cancer. Surgery involves operations to remove ovarian cancer and these may include:
Removal of only the affected ovary and its fallopian tube. This usually applies to the very early stage cancer that hasn’t spread beyond one ovary. This procedure may preserve a woman’s ability to have children.
Surgery to remove both ovaries and their fallopian tubes. This is applicable if the cancer is present in both ovaries, but there are no signs of additional cancer in any other part of the body. This procedure leaves the uterus intact so that the woman will still be able to become pregnant using frozen embryos or eggs or eggs from a donor.
Removal of both ovaries and the uterus. This is the preferred surgical procedure, when the cancer is more extensive or if the woman does not wish to preserve her ability to have children.
Chemotherapy is recommended for women with ovarian cancer after surgery. Chemotherapy is a drug treatment that uses chemicals to kill fast-growing cells in the body, particularly cancer cells. These drugs can be injected into a vein or taken by mouth. Sometimes, the drugs can be injected directly into the abdomen (intraperitoneal chemotherapy). Chemotherapy is often used after surgery to kill any cancer cells that might remain. It can also be used before surgery for advanced cancer to enable the removal of as much of the ovarian cancer cells as possible.
What should women know about screening?
There is a consensus that screening for ovarian cancer in the general population of women, without symptoms or any major risk factors, is not recommended. However, the recommended screening tests for symptomatic or high-risk women (with inherited gene mutations or family history of ovarian cancer) may include transvaginal ultrasound and blood CA-125 testing, in addition to physical examination.
What should be done to reduce the risk of ovarian cancer?
There’s no sure way to prevent ovarian cancer from occurring. But there may be strategies for reducing the risk of getting the disease. Some of these strategies include:
The use of birth control pills – Women who use oral contraceptives may have a reduced risk of ovarian cancer. But oral contraceptives also have risks, and it is important that women know the benefits against these risks, based on their situation.
Women with a family history of breast and ovarian cancers should bring this up with their doctors. The doctor can determine what this may mean for a woman’s risk of getting ovarian cancer, and the doctor may consider it necessary to refer such a woman to a genetic counselor, who can help to decide whether genetic testing may be needed. If a woman is found to have a gene mutation that increases her risk of ovarian cancer, she may consider surgery to remove her ovaries to prevent cancer.
 Follow Us on Google News
Follow Us on Google News
 Follow Us on Google Discover
Follow Us on Google Discover
