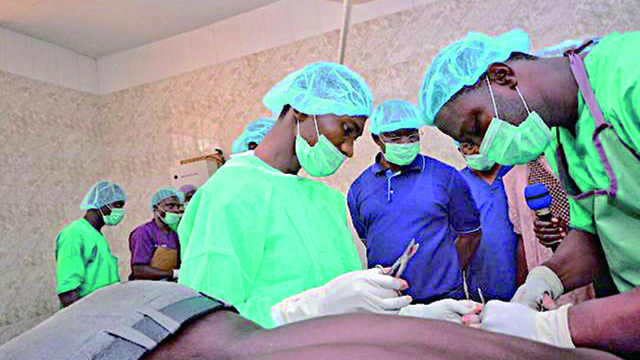
Nigerians have ushered in the year 2020 with fresh and high hopes that the Federal and State Government would provide improved, quality and affordable healthcare for all.
Although, President Muhammadu Buhari had presented the proposed 2020 budget of N10.33 trillion, the health sector received 4.14 percent, that is, N427.03 billion, out of the total budget.
However, there was an increase in the recurrent expenditure from N315.62 billion in 2019 to N336.32 billion in 2020, while there was a shortfall in the capital expenditure from N50.15 billion in 2019 to N46.48 billion in 2020.
Also, the Basic Health Care Provision Fund (BHCF) has been on a downward progression since the first allocation of N55.15 billion in 2018. In 2019 about N51.22 billion was earmarked and the lowest in 2020 with N44.498 billion.
Other projects included in the 2020 proposed budget for health that also experienced a decline, apart from the slight increase in the N44.50 billion provisioned for the implementation of the National Health Act include:
• N22.73 billion provided for GAVI/Immunisation
• N4.8 billion Polio Eradication Initiatives
• N815 million for the procurement of Non-Polio SIA Vaccine
• N655 million for the procurement of Kits And Commodities For Community Health Influencers
• N2 billion for expanded midwives service scheme
• N5.5 billion for counterpart funding including global fund/health
• N4 billion for Procurement of RI Vaccines & devices
Stakeholders in the health industry have lamented that the monies fall short of what is needed to meet the needs of the country’s health sector.
They have, however, set the agenda for health in 2020, while calling for improvement and strategic measures to ensure Nigeria achieves universal health coverage.
The stakeholders who spoke to The Guardian include President, Nigerian Medical Association (NMA), Dr. Francis Adedayo Faduyile; President, Pharmaceutical Society of Nigeria, (PSN), Mazi Sam Ohuabunwa; Senior Registrar, Department of Preventive Dentistry, Lagos University Teaching Hospital (LUTH), Dr. Ekowmenhenhen Uyi Idah; Chairman, Medical Advisory Committee, LUTH, Prof. Wasiu Lanre Adeyemo; President, Association of Psychiatrists in Nigeria, Taiwo Lateef Sheikh; Registrar, Department of Anaesthesia, Federal Medical Centre, Ebute Metta, Dr. Olaoye Oludare and Head of Legal Department, Lagos University Teaching Hospital, Sesan Olajide.
They said to achieve universal health coverage and improve the health of citizens in the country, there must be more focus on funding, health insurance, manpower, adequate equipment and infrastructure, drug security, the passage of health bills, and a reduction in mortality, among other recommendations for healthcare in 2020.
Increase coverage of the National Health Insurance Scheme (NHIS)
Faduyile said the NHIS, which was established in 1999 with the commencement of operation in 2005, is yet to deliver on its mandate and appears to be far from affecting a paradigm shift soonest.
“It is no news to state that the performance of the scheme is largely abysmal with less than five per cent of the population covered. The poor performance has been attributed to many factors ranging from poor funding to lack of transparency in its administration.
“The Governing Council of NHIS noted the following as key to the failure experienced so far: a decline in remittances, persistent budget deficit, management fiscal indiscipline, conflict and corruption.
“With the provision of the one per cent Consolidated Revenue Fund (CRF), a significant source of the Basic Health Care Provision Fund (BHCPF) for which 50 per cent is supposed to be disbursed through the NHIS, in the 2018 budget, it has become a must to nip the challenges encountered so far in the bud for Nigerians to benefit reasonably from Basic Health Care that the fund is meant for. The Federal Government/Federal Ministry of Health (FMoH), NHIS, Health Maintenance Organisations (HMOs), Health Service Providers (HSP), enrollees, civil society organizations, professional bodies in the health sector including the NMA, must rise to the occasion and synergize appropriately.
He continued: “Few States are now starting their own version of the scheme without involving critical stakeholders like NMA. The states governments have largely politicised the State Health Insurance Scheme in their respective state. Although, we want all States to come on board the proper process should be followed, otherwise, it will not be sustainable. The Federal and State Governments should also bring a template for the inclusion of the non- formal sector-the farmers in the village, pretty traders among others in the scheme. There is also a need to review the current operational strategies of the scheme and ensure that all the relevant stakeholders are on the same page.
To improve the health sector, Ohuabunwa, said the Federal and State Governments should enforce health insurance at all levels, as those who are poor should receive support in the form of subsidy.
“Let 2020 be the year of Universal Health Insurance coverage in Nigeria”, noting that there is no significant increase in national health insurance coverage, as most Nigerians still purchase medicare out-of-pocket that would have caused much morbidities and mortalities.
Professor of Virology, Oyewale Tomori said: “We must find ways to make the National Health Insurance Scheme (NHIS) truly covering the majority of our population.”
Adequate funding and budgetary allocation to health
Tomori said Health Development Fund should be spent on equipping existing health facilities, “so we can focus on Primary and preventive healthcare nationally.”
Senior Registrar, Department of Preventive Dentistry, Lagos University Teaching Hospital (LUTH), Dr. Ekowmenhenhen Uyi Idah, said: “With the budgetary allocation, even if there is a slight increase, it is still not much. I don’t expect anything fantastic, it will just be marginal increase or advancement on last years performance, which underscores the fact that there has to be a greater commitment because health is one of the basic and fundamental rights of humans and any serious government must place it as a priority alongside education, housing and other basic rights.
“All these things have an interconnectedness or a nexus in promoting the wellbeing and health of the individual in its entirety.
Sheikh said there should be adequate funding of mental health services and provision of psychosocial support services to persons living with mental and psychosocial disabilities, with a view to guaranteeing their mental wellbeing; protecting their fundamental human rights and ensuring social inclusion.
Oludare, said as the country has stepped into a new year, efforts should be geared towards making the health of high priority, as well as ensuring equity in budgetary allocation towards the health sector.
Faduyile urged the federal and state governments to: “Increase budgetary allocation to meet 15 per cent of the total budget, universal health coverage for all Nigerians, improve work environment in our hospitals and upgrade of the infrastructure to meet international standards in order to reverse medical tourism, immunisation particularly, strengthening polio virus immunization, surveillance and monitoring before the anticipated declaration of Nigeria free of Polio virus in August this year, strengthening of National Health Insurance Scheme (NHIS), State owed health insurance Scheme and Community Insurance Scheme to ensure qualitative services delivery, promoting industrial harmony in the health sector.
He continued: “Improve welfare conditions of all health workers in Nigeria, ensuring that the one per cent of the Consolidated Revenue Fund of the federation in the 2018 budget already released for properly utilised for improved funding of primary healthcare in Nigeria as mandated by the National Health Act 2014, to capture more Nigerian and putting strategies in place to curtail the emergence and re-emergence of viral haemorrhagic diseases and epidemic diseases in Nigeria.”
Resolve brain drain and improve the reward system
Faduyile had stressed Nigerian doctors and other healthcare workers, including nurses and pharmacists, are leaving the country in droves, noting that only 42,000 doctors out of the 75,000 registered by the Nigeria Medical Association (NMA) are available for Nigeria’s 200 million people.
He said the 33,000 missings, have left for greener pastures, further attributing the emigration of Nigerian doctors to high rate of insecurity, poor job satisfaction, low remuneration, unemployment, bad roads, and the poor healthcare system.
He further revealed that to buttress country’s the collapsed health care system the ratio of doctor to patients in rural areas is 1:22,000, while in towns and cities, is 1:10,000 or 1:12,000, which is contrary to the World Health Organisation (WHO) ratio for countries, which is, one doctor to 600 persons.
“The United Kingdom employs, on average, 12 Nigerian doctors every week. If Nigeria decides to graduate 3,000 doctors every year, without the doctors leaving this country, it will take us 25 years to meet the WHO estimate of one doctor to 600 persons.
He continued: “This has a negative effect on the economics of developing countries, because the skills of remaining professions may not be adequate to grow the economy. This is apart from the fact that the health needs of the population cannot be met due to reduced number of health personnel. The remuneration of health workers are very poor in this country and health workers take home in Nigeria is about 30 percent of what their colleagues are being paid abroad. The reward system is so bland that most health workers see nothing that is keeping them happy. There are no opportunities for car loan, housing loan and special allowances as applicable to their colleagues working abroad. All these contributed significantly to the on-going mass exodus of health workers.
Ohuabunwa said the government must ensure massive employment and competitive compensation of health personnel to ensure that no health institution operates without adequate professional manpower.
Oludare said the government must make deliberate efforts to preserve and utilise human resources by providing conducive and comfortable working conditions.
Sheikh said: “There is an urgent need for the recruitment of mental health professionals into all levels of healthcare delivery service. As mental health is inseparable from physical health, adequate provision should be made for the training of all healthcare personnel on basic mental health and psychosocial skills for effective task sharing and task shifting generally and specifically.
Drug insecurity, abuse and misuse
For safety and drug security, the Faduyile, said: “It is important to state that winning the war against issues surrounding drug insecurity will not be only by such action but requires the deployment of strategies centered on Prescription Rights. The enforcement of Prescription Rights will ensure that only with a prescription from a doctor would a pharmacist dispense such drug(s).
“The government should ensure more security measures are put in our borders to guide against the importation of these drugs, work more on how to halt the distribution lines as well as educating the youth on the evil of drug abuse. “Another dimension to drug insecurity is the unnecessary and wasteful spending on drugs like antibiotics in a society with poor per capital income. Apart from its capability to worsen poverty, it also leads to the development of drug resistance especially in the case of antibiotics and antimalarial.
“In this 2020, government and its agencies must ensure the enforcement of prescription rights and the monitoring of the distribution and dispensary of drugs especially at dispensary outlets.”
Ohuabunwa said the government must reintroduce the drug revolving fund schemes in all tertiary health institutions to assure continuous access of essential medicines.
Increasing public-private partnership
Idah called for: “Inter-sectoral collaboration, constant partnership and a purposive commitment on the side of the government – incorporating the private sector to ensure we actually advance the course of the health sector in Nigeria.”
Adeyemo, said Nigeria must strengthen its public-private partnership, adding, “I expect that we continue the trajectory – combining the opportunities of the public hospitals and those of private people who have the money to invest so that healthcare delivery in Nigeria can be better.”
Olajide said the government needs to improve capacity in terms of infrastructure, equipment and training, noting that the way to go is a public-private partnership, which should be properly managed, in terms of training practitioners to take care of health in general.
He said if this is done, “definitely our health system has the capability to withstand or compete with any health system all over the world.”
Passage of all health bills
Sheikh urged the government to ensure the passage of the Nigeria Mental Health Bill into law, as it will comprehensively address substance abuse challenges in the country.
“It will also regulate mental health and substance abuse services, and the establishment of National Commission for Mental Health and Substance Abuse Services for effective management of mental health and psychosocial disabilities and other related matters in Nigeria.”
Other measures, Ohuabunwa said the government must take, include: “Progress the plan to establish at least four centres of medical excellence in Nigeria to stem medical tourism and restore National prestige, as well as pass all outstanding legislations, especially the Pharmacy Bill to help improve regulation and sanitise our drug distribution system.”
 Follow Us on Google News
Follow Us on Google News
 Follow Us on Google Discover
Follow Us on Google Discover