What is vitamin D?
Vitamin D is organic fat-soluble vitamin, which is essential for normal metabolic processes, especially related to mineral and bone metabolism.
This means that vitamin D essentially helps the body to absorb calcium, magnesium and phosphorus, when ingested and then made to attach adequately to the bone to allow for good skeletal structure, and some other body processes to function well.
The human body is unable to produce it from scratch and so requires some external factors like ultra-violet radiation from the sun and a balanced diet before adequate and active form of vitamin D can be produced in the body.
Vitamin D exists in different forms as active and inactive forms, which include cholecalciferol D3 and ergocalciferol D2.
These forms are converted to the active form of vitamin D referred to as 1, 25, dihydroxy cholecalciferol.
Vitamin D is required for proper bone and mineral metabolism together with parathyroid hormone to control absorption, metabolism and excretion of calcium, phosphorus and magnesium.
These minerals are essential for development and maintenance of strong bone and musculoskeletal structure and function.
Apart from sunlight, what are the sources of vitamin D and how much does the human body need?
The ultraviolet part of sunlight is essential for the body to synthesise the precursor forms of vitamin D cholecalciferol D3.
Ergocalciferol D2 is photosynthesised in plants and can be taken as diet.
These forms of vitamin D are metabolised in the liver and kidneys to the active form of vitamin D through which most of the metabolic effects are achieved.
Dietary sources of vitamin D include, liver oil, fatty fish, egg yolk, liver, fortified yoghurt, cheese and some juice products.
Also, vitamin D is got through supplements, which have been engineered with fixed dose of vitamin D in various forms.
The recommended daily allowance for vitamin D intake ranges from about 200 to 1000 international units per day.
In deficiency states, the daily intake can be as much as 2000 international units. Children and adults up to the age of 50 need 200IU vitamin D per day.
Adults aged 51 to 70 need 400 IU vitamin D per day, and those aged more than 71 require 600 IU vitamin D daily.
Post menopausal women, the obese, and those with fat malabsorption or other risk factors need 800 to 1000 IU vitamin D per day.
How is the level of vitamin D in the body determined?
In a normal growing child or healthy adult, it is assumed that vitamin D metabolism is normal and adequate.
However, pathological conditions may require that the level of vitamin D and the different metabolites be determined through the laboratory and adequately interpreted by qualified medical personnel.
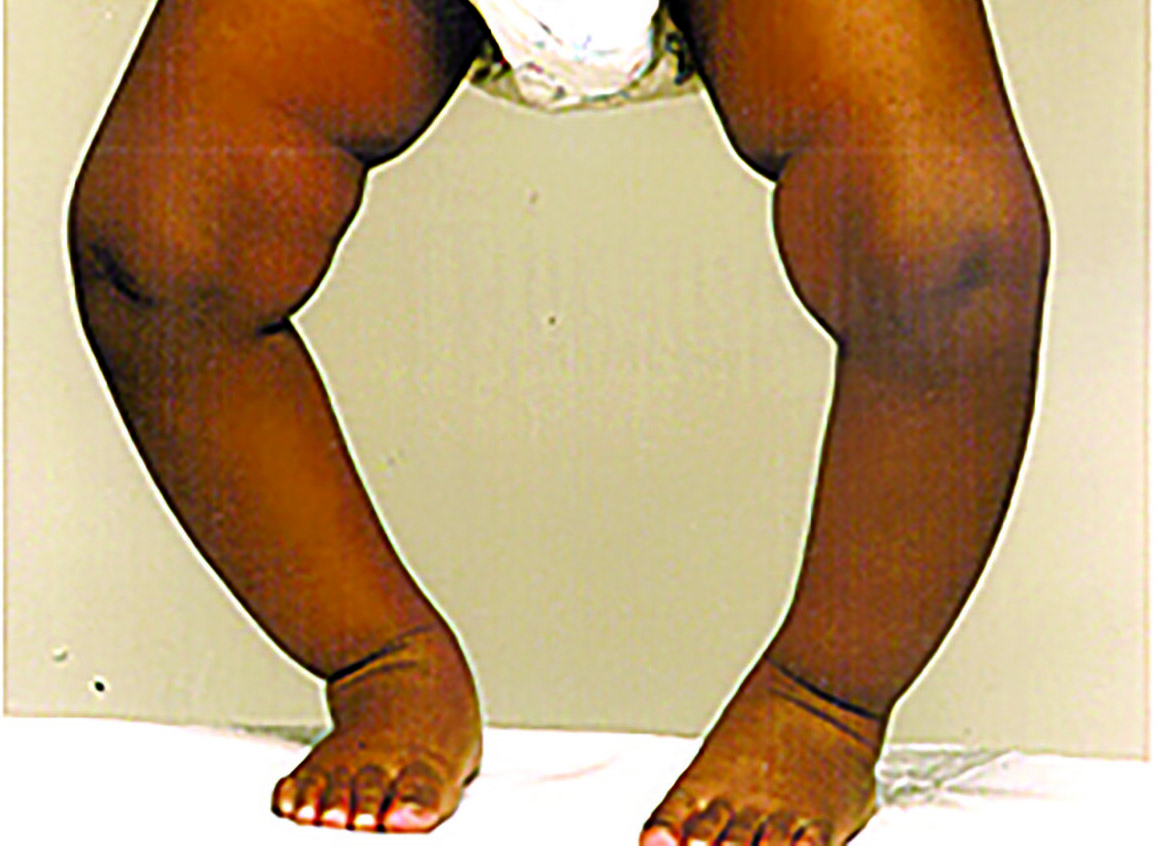
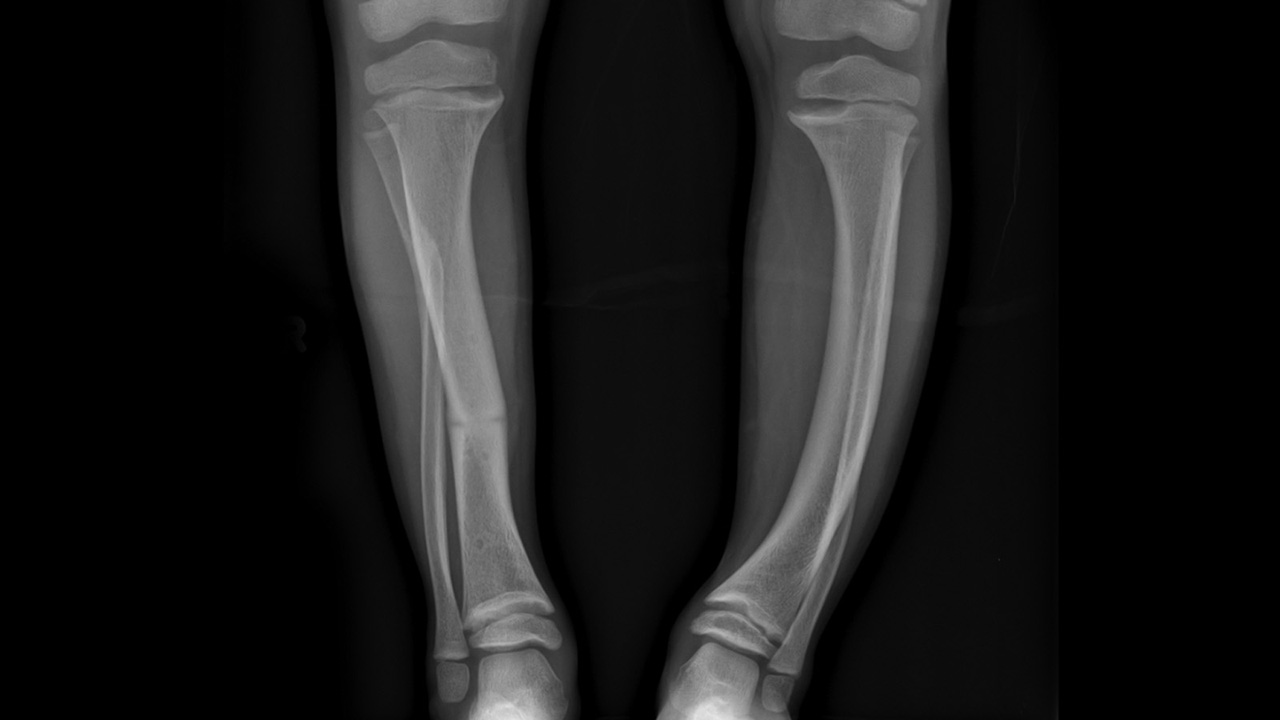
Pathological states include, poor or stunted growth in children, recurrent chest infections, development of bow or knock-knees in children (Rickets), delayed development milestones in children, osteomalacia orosteoporosis in adults, muscle weakness or pain and poor cognitive functions.
Also, parathyroid hormone, calcium, magnesium and phosphate blood levels need to be assayed.
What are the causes of vitamin D deficiency?
Malnutrition, which can be due to ignorance of parents/guardians on provision of balanced diets or poverty, non-provision of adequate exposure to sunlight, genetic/hereditary conditions, which may cause inability of the body to produce active form of vitamin D or the body not being able to adequately respond to the presence of active vitamin D.
There are also such pathological states as chronic kidney disease and chronic liver disease and use of drugs, which interfere with vitamin D metabolism like rifampicin, dexamethasone and some anticonvulsant medications.
What symptoms and consequences can be associated with vitamin D deficiency?
Poor bone formation and structure, poor neuromuscular and nerve functions, increased risk of developing bone deformities like rickets in children and osteomalacia in adults, increased incidence of neuropathic pain in individuals with type 2 DM, increased risk of developing such autoimmune disease states as multiple sclerosis, rheumatoid arthritis and type 1 DM and may contribute to increased risk of developing such cancers as colorectal cancer and leukemia.
What groups are most at risk of vitamin D deficiency?
Children, elderly, house-bound and nursing home residents, obese individuals who store more of the inactive vitamins in adipose tissues, women on oral contraceptives.
Others include individuals with pathologies like malnutrition, chronic liver or kidney disease, as well as pregnant women.
What happens to the body, if there is excess vitamin D?
It is unusual for excess of vitamin D to occur in the body, because there is a negative feedback mechanism, which downplays the processes involved in absorption and conversion to active vitamin D.
Exogenous intake of vitamin D, either through regular intake of vitamin as supplements, or through therapy may cause hypervitaminosis.
A high level of vitamin D above a defined cut off (above 150 to 200 ng/ml) is associated with increased amount of calcium in the blood.
This high level of calcium is what causes the damages associated with high level of vitamin D in the body, affecting the bone, cardiovascular system and enzymatic activities in the body.
Noted signs and symptoms include, general body weakness, weight loss, confusion, poor concentration, drowsiness, nausea, vomiting, depression, abdominal cramps and in extreme case, may lead to coma.
It may also cause a condition called nephrogenic diabetes insipidus in which the body is unable to store water, causing the individual to continually pass a lot of urine.
Excess calcium in blood also puts the individual at risk of developing kidney stones, which may cause kidney pains and kidney failure.
Management of high vitamin D in the body involves discontinuation of vitamin D intake, restriction of calcium in diet, use of steroid and other specific treatments to control the effects of excess calcium in the blood. Vitamin D toxicity is not a common occurrence compared to vitamin D deficiency.
What home remedies are available to manage vitamin D deficiency?
Prevention is better than cure. Sunshine is readily available. Morning sunshine bath is advised for individuals at risk for about 30 minutes to an hour per day.
The use of sunscreen creams on the skin significantly reduces the capacity of the skin to produce vitamin D.
Vitamin D rich food includes cod liver oil, fish (such as mackerel, sardines, catfish), egg, and green vegetables.
Fortified food products are readily available and children especially can be placed on diets with good source of vitamin D. Milk and dairy products, bread, yoghurt, soy products and cereals.
Suspected cases of vitamin deficient individuals should see qualified medical personnel for investigation and management, especially after failure to respond to available local remedies.
[ad unit=2]
 Follow Us on Google News
Follow Us on Google News
 Follow Us on Google Discover
Follow Us on Google Discover