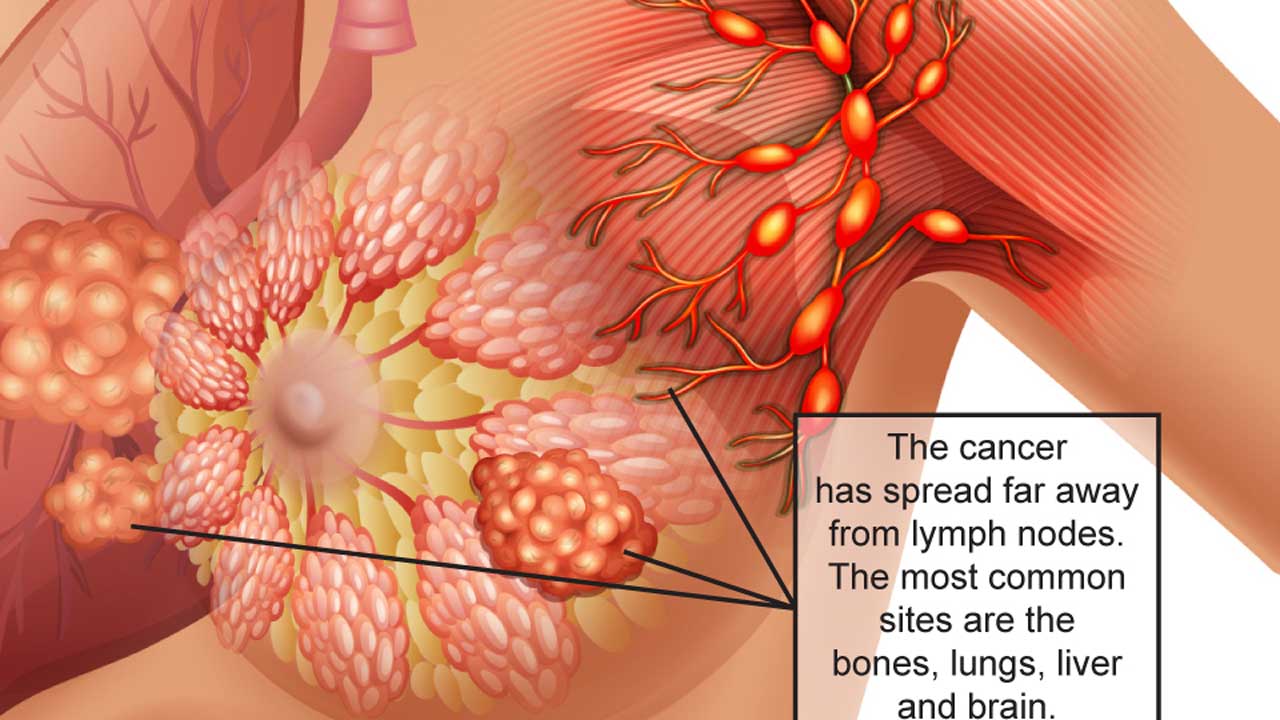
Experts in oncology have said to improve breast and cervical cancer care and treatment as well as reduce its prevalence in Nigeria, delay in the presentation must be tackled at all levels.
They gave the submission during the Society of Oncology and Cancer Research of Nigeria (SOCRON) three-day conference on Multidisciplinary Cancer Management Course (MCMC), in collaboration with the American Society of Clinical Oncology (ASCO), with the theme: “Implementation of Resource Level Appropriate Breast and Cervical Cancer Prevention, Diagnostics and Management.”
The team of experts lamented that the incidence of breast and cervical cancer in Nigeria keeps increasing due to lesser number of women presenting early in the hospitals, as well as other factors, which include: unavailability of funds to drive treatment, fewer medical manpower, lack of cancer centres, equipment and machines, and delay in diagnosis at public hospitals, as well as patients attitudes and beliefs.
Professor of General Surgery, Breast and Endocrine, University of Abuja Teaching Hospital, King David Terna Yawe, in his presentation titled: “Delayed Presentation and Clinical Features of Breast Cancer in Nigeria”, said many of the factors affecting positive cancer care in Nigeria include: the location of the patients in rural communities, inadequate facilities and experts to attend to them as well as the potent issues of money, as patients have to pay for treatment and other healthcare services in the hospital, describing it as a “cash-and-carry system”.
He said the government needed to expand the health facilities, providing more clinic space as well as have more availability of time and resources to attend to more patients among the huge Nigerian population. Yawe, who is also the Vice President, SOCRON, stressed the need to address the issue of cancer care in Nigeria with a more robust health insurance policy that covers everybody, noting that at the moment, the health insurance scheme involves just about five percent of the population and practically mostly civil servants. He also added that to achieve total coverage of all Nigerians, the government must explore community-based health insurance system if we want to cover a bulk of the population.
Yawe said cancer care should be added as primary healthcare, noting that bulk of the population resides at that local level and that the minimal examination of a patient does not have to be done in a specialist hospital if the primary health system is working well, which could be a veritable source of referral.
“We are also treating breast cancer as a community health problem, so we should first commence dealing with that matter in the community. Primary health centers are for early screening and breast examination, it doesn’t require anything than the hand, which is why I am advocating that we can pick them a bit earlier and then they are sent to the referral centers where they can be attended to,” he stressed.
Lamenting on the inadequate manpower in the medical field, Consultant Gynaecologist and Obstetrician, Dr. Bunmi Alabi, stressed that a hospital abroad, where many Nigerian doctors practice has about 400 bed spaces, with 37 pathologists to attend to patients, whereas, Nigeria with its huge population of over 200 million has less than 200 pathologists.
He said this puts the ratio of the pathologist to patients at 1:1,000,000, noting that the government should train more hands in the profession and provide an enabling working environment to have more specialists attend to patients.
Also speaking on training manpower as effective measure to achieve success in cancer care, the Director of the Breast Health Global Initiative of the Fred Hutchinson Cancer Research Center, Dr. Benjamin Anderson, said, “In terms of early detection, we found that part of the problem could be that the primary care clinicians that first met the patient do not really know what breast cancer is like and so they send the patients away rather than doing a diagnostic workup. Sometimes the surgeons will make a mistake, they will cut out cancer and throw it away. Cutting it out only removes the problem, but it doesn’t tell you how to treat it…”
You have to analyze the tumor, figure out what type of breast cancer it is and then provide the treatment.”Anderson, who is also a Professor of Surgery and Global Health–Medicine at the University of Washington School of Medicine in Seattle said the responsibility of positioning addressing the problems in the Nigeria health system rests on the government, the health ministries and other stakeholders, as no foreign could do that for the country.
Speaking on the benefit of the conference, the President of SOCRON, who is also a Professor of Surgery, University of Ibadan, Clement Adebamowo, said it is for stakeholders to appreciate that there is now enough scientific knowledge about how to reduce death from the many types of cancer, which are not been applied in Nigeria.
The Professor of Epidemiology, University of Maryland School of Medicine also commented on the implementation of the National Cancer Control Plan 2018-2022, saying, though, government should be congratulated for coming up with the policy, the Executive arm of the government and the legislature need to work together to provide funds and resources needed to back it up from being just a policy on paper.
 Follow Us on Google News
Follow Us on Google News
 Follow Us on Google Discover
Follow Us on Google Discover
