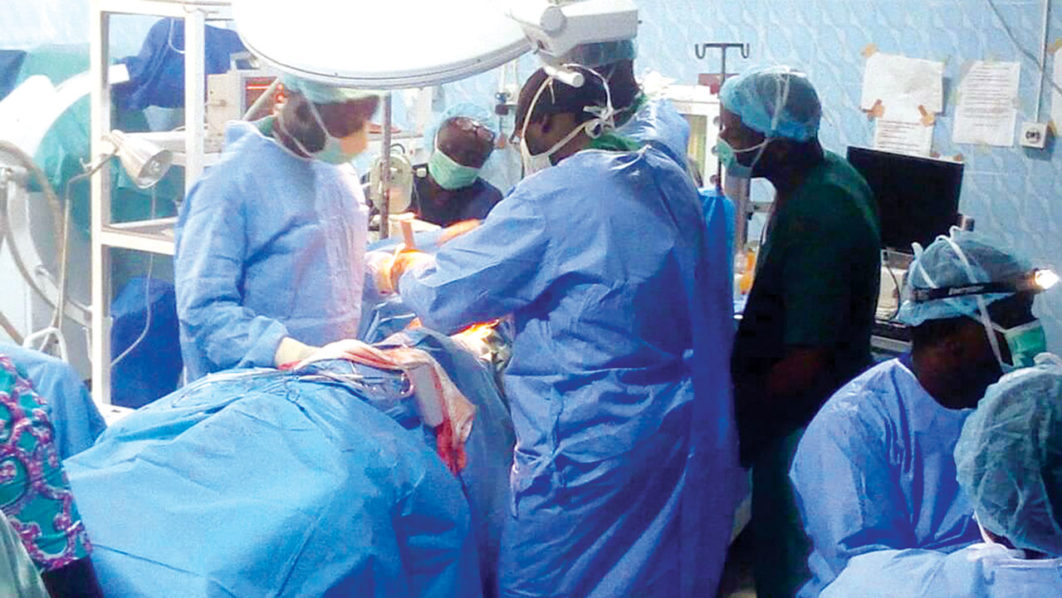
In separate interviews with The Guardian, they shed light on the urgency of the situation, calling on the Federal Government to do more to save the nation’s health infrastructure.
It is estimated that at least 2,000 medical doctors leave the country yearly for the United Kingdom, United States, Canada, Australia, United Arab Emirates (UAE), and South Africa.
“This is cataclysmic, given the fact that currently, contrary to the recommendations of the World Health Organisation (WHO) of a ratio of one doctor to 600 patients, Nigeria has a ratio of one doctor to 6,000 patients.
This poor doctor-patient ratio is regrettable when compared to the ratio of doctor to patients in India (1:2083) and in the United States (1:500).”
Figures released February 2018 by the British government indicate that no fewer than 5,405 Nigerian-trained doctors and nurses are currently working with the British National Health Service (NHS) in the United Kingdom (U.K.).
This means that Nigerian medics constitute 3.9 per cent of the 137,000 foreign staff of 202 nationalities working alongside British doctors and nurses.
A Consultant Neurological Surgeon, Brain and Spine Surgery Consortium Abuja, Dr. Biodun Ogungbo, regretted that fresh doctors no longer see a bright future within the shores of Nigeria. “The conditions of work are poor.
The facilities are poor and the remunerations are poor. Many doctors are breadwinners in their families but are unable to deliver family expectations,” he said.
He advised: “The government needs to take healthcare seriously and make it a major priority in view of its critical importance to our lives. The amount budgeted for health must be increased. Better financing translates to more remuneration for health workers, increased training opportunities for doctors, availability of equipment and other consumables.”
Professor of Radiology, College of Medicine, University of Nigeria Nsukka, Ifeoma Okoye, shared her experience on the pitiful state of the healthcare system: “As a radiologist, my colleagues and I have faced frustration and embarrassment due to lack of imaging equipment to hone our skills and provide quality service confidently to our patient population, as well as hold our heads high at international fora, where we are faced with colleagues who run their daily practice on the latest high-end modalities.
For most of us, knowledge of such equipment is at best theoretical and these experiences of inadequacy turn our professional lives into one of hard labour and frustration.”
Okoye, also a Consultant Radiologist, University of Nigeria Teaching Hospital Enugu
(UNTH), explained: “Trained health professionals are needed in every part of the world, and so when healthcare professionals lack opportunities for professional development, enabling environment to practice and optimise their skills, and find that their quality of life and ability to train their children in the best educational institutions is gated by their poor salaries (compared to their peers in more advanced countries), they permit their brains to be drained.”
According to her, developing the clinical trial industry can add value to “identified growth indicators and become the cornerstone of health and economic transformational agenda, which should help Africa climb up the value chain towards industrialisation and provide opportunities to bring the large informal sector progressively into the formal economy.”
Dr. Muhammad Ali Pate, former Minister of State for Health and Executive Director Primary Health Care Development Agency (NPHCDA), told The Guardian: “If political leaders, who control the public purse, continue to choose to travel abroad for medical care, it is a signal for domestic health workers that they, too, ought to travel abroad, in order to practice and advance themselves professionally. We cannot have one without the other.”
His view was shared by Medical Director and Chief Executive Officer, Beaconhill Smile Clinics, Dr. Oluwaseun Akinbobola, who noted: “Healthcare is not a priority in our nation, as most decision makers would rather travel abroad when the need arises. Until we prioritise healthcare, I don’t believe this dramatic exodus of doctors will end. You cannot fix a health system you don’t believe in.”
He, therefore, advised: “The leadership of the country must instill confidence in and show willingness to improve healthcare services by signing necessary health acts and bills, increasing funding for the sector and ensuring that funds are properly managed.”
Former President of the Nigerian Medical Association (NMA) and Vice President Commonwealth Medical Association (CWMA), Dr. Osahon Enabulele, recommended: “Better political commitment to health; better appreciation of the worth of medical personnel, along with better and competitive wages; better working conditions and inspiring work environment; better security and access to social amenities; attractive and globally respected postgraduate training programmes.”
Medical Director, Optimal Specialist Hospital Surulere, Lagos, Dr. Celestine Ugochukwu Chukwunenye, on his part, stressed: “Federal Medical Centres should be handed over to the states. Each teaching hospital should then be allowed to float or sink.
Their governing boards should reflect the interest of their catchment area and appropriate pricing of their services in line with available government subsidies.”
He said the National Health Insurance Scheme (NHIS) must be strengthened to provide better access to these facilities. According to him, it is a ruse to think that forcing the teaching hospitals to charge fees like Primary Health Centres (PHCs) is the way to improve access to them.
Patients, meanwhile, have deserted the University of Calabar Teaching Hospital (UCTH), following the strike action by members of the Joint Health Sector Unions (JOHESU), now in its fourth day.
The union embarked on the strike after the expiration of an ultimatum it gave the Federal Government, alleging non-implementation of an agreement that included salaries.
[ad unit=2]
 Follow Us on Google News
Follow Us on Google News
 Follow Us on Google Discover
Follow Us on Google Discover

