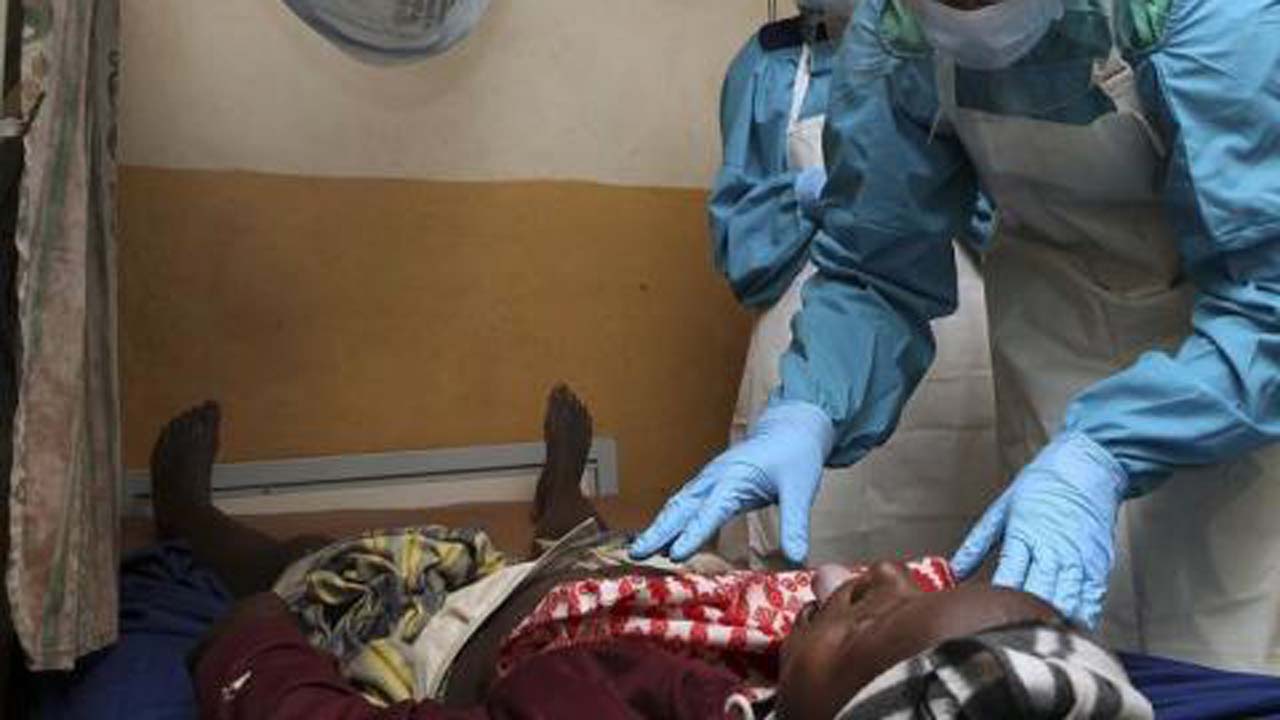
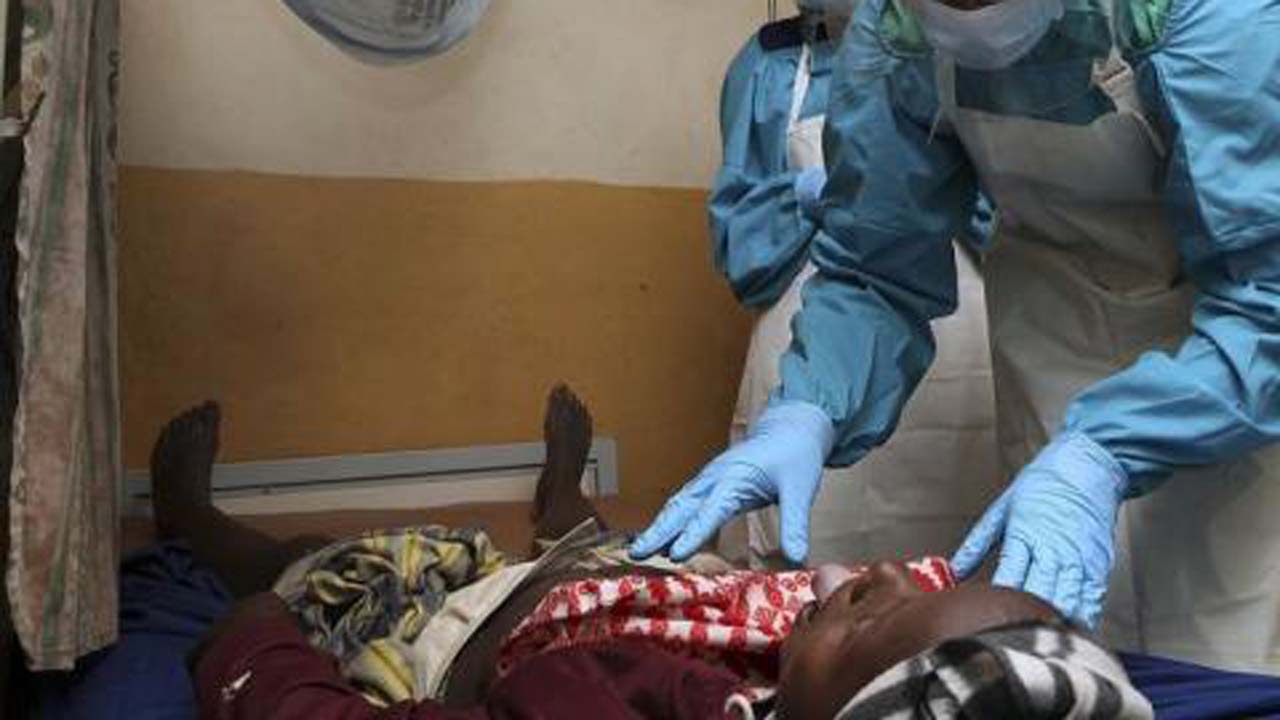
 The annual resurgence of Lassa fever in the country should be a major source of worry to health authorities as reports from some parts of the country are alarming. Not only is the fatality from the ailment increasing, health workers are also dying of the disease they are to cure. Notwithstanding the surge in coronavirus infections, Lassa fever should be treated as an emergency to halt needless morbidity and mortality in Nigeria.
The annual resurgence of Lassa fever in the country should be a major source of worry to health authorities as reports from some parts of the country are alarming. Not only is the fatality from the ailment increasing, health workers are also dying of the disease they are to cure. Notwithstanding the surge in coronavirus infections, Lassa fever should be treated as an emergency to halt needless morbidity and mortality in Nigeria.
Lassa fever is an acute febrile illness, with bleeding and death in severe cases. According to the World Health Organisation (WHO), it is an acute viral haemorrhagic illness of 21 days duration that occurs in West Africa.
Descriptions of the disease date from the 1950s, but it was first described in 1969 from a case in the town Lassa, in Borno State, Nigeria. The virus is zoonotic, or animal-borne. The WHO states that the reservoir or host of the Lassa virus is the “multimammate rat” called mastomys natalensis, which has many breasts and lives in the bush and around residential areas. So, it is mostly spread by rats.
The virus is shed in the urine and faeces of the rats hence can be transmitted to humans via direct contact, touching objects or eating food contaminated with these materials or through cuts or sores. Person-to-person infections and laboratory transmission can also occur, particularly in hospitals lacking adequate infection prevention and control measures. Persons at greatest risk are those living in rural areas where mastomys are commonly found, especially in communities with poor sanitation or crowded living conditions.
About 80 per cent of human infections are without symptoms; the remaining cases have severe multiple organ disease, where the virus affects several organs in the body, such as the liver, spleen and kidneys. When it is symptomatic, the onset is gradual, starting with fever, general weakness, muscle and joint pains, prostration and malaise. After a few days, headache, sore throat, muscle pain, chest pain, nausea, vomiting, diarrhoea, cough, and abdominal pain may follow. In severe cases, facial swelling, fluid in the lung cavity, bleeding from the mouth, nose, vagina or gastrointestinal tract and low blood pressure may develop. Shock, seizures, tremor, disorientation, and coma may be seen in the later stages.
According to the Nigeria Centre for Disease Control (NCDC) in its latest Sitrep on the outbreak of the disease in the country, the death toll for Lassa fever in Nigeria from January 2021 has risen to 92 with Bauchi and Ebonyi states recording new deaths, with a Case Fatality Rate (CFR) of 20.3 per cent. Out of a total of 190 new cases suspected in 11 states and the Federal Capital Territory, 10 cases were confirmed in four states; two of them being healthcare workers.
In all, as of the reporting Week 50, a total of 454 people have been infected by the disease across 66 Local Government Areas in 16 states of the federation and the Federal Capital Territory (FCT). Out of all confirmed cases, Edo has (43 per cent), Ondo (35 per cent), and Taraba (five per cent). The predominant age group affected is between 21 and 30 years. Although the number of suspected cases has decreased compared to that reported for the same period in 2020, the trend of cases and infections has persisted over the past six or seven years.
Obviously, Lassa fever is a health deficit in Nigeria that cuts across class; it requires practical and strategic credits to nil the account! However, this situation does not call for panic as early supportive care with rehydration and symptomatic treatment improves survival chances. As such, the affected State Ministries of Health and the Federal Ministry of Health should respond to contain the current Lassa fever outbreak by mobilising human and material resources to trace the sources and extent of the disease, follow up on potential contacts, identify early and test suspected cases.
In view of the fact that health authorities are already stretched by COVID-19 crisis, all hands must be on deck to redress this situation. Strategically, since there is currently no vaccine that protects against Lassa fever, prevention is the key. Its prevention relies on scientific interventions, societal and individual behavioural changes hinged on good hygiene. Individuals should learn to store grains and other foodstuff in rodent-proof containers, dispose of garbage far from the home and maintain clean households. Health workers should maintain a high level of alert in the wake of this new outbreak and observe universal precautions in handling all suspected cases of this viral haemorrhagic fever.
The scientific intervention requires that the Federal Ministry of Health, Centre for Disease Control (CDC) in Nigeria, Nigerian Institute of Medical Research, Institute of Human Virology, Nigerian research and development units of health-related organisations such as pharmaceutical companies and universities should collaborate and engage in a well-coordinated manner to search for solutions, through research on the specie of rat that hosts the Lassa virus and how to make them de-zoonotic in order to render them impotent as carriers. They should also lead a vaccine and treatment research, particularly now that the federal government recently said that Nigeria is set to resume local production of vaccines after 27 years.
Finally, the virology centre built by the Ebonyi State government some years ago should be made fully functional; to reduce the unnecessary and arduous ferrying of victims of Lassa fever from the east, by road to Irrua in Edo, a process that often leads to death from exhaustion of some victims.
 Follow Us on Google News
Follow Us on Google News
 Follow Us on Google Discover
Follow Us on Google Discover