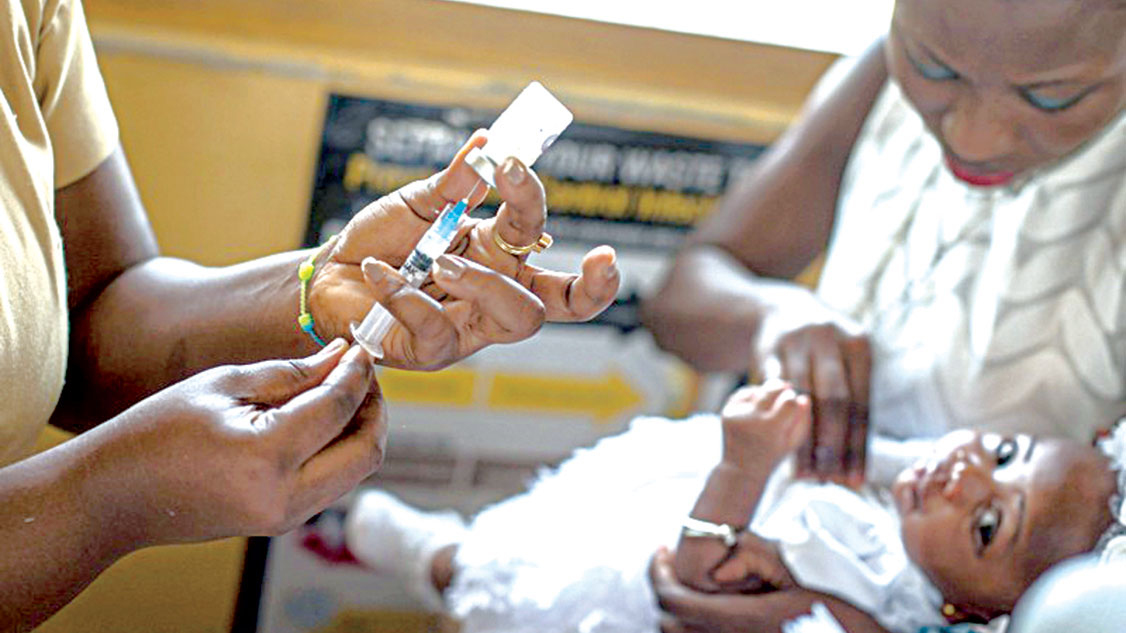
With the recent endorsement of the long-expected first malaria vaccine, RTS, S/AS01 (RTS,S), by the World Health Organisation (WHO), children in sub-Saharan Africa and in other regions with moderate to high Plasmodium falciparum transmission will, for the first time, get a respite from deadly malaria affliction. For a disease that accounts, yearly, for the death of no fewer than 260,000 African children under the age of five, malaria is a terrible scourge that is capable of wiping out a whole generation of Africans if unchecked. For this reason, this vaccine is a laudable health security game changer. But a lot still needs to be done as the vaccine alone will neither exterminate malaria nor eliminate malaria-induced challenges particularly for adults.
According to reports, the endorsement came from results of an ongoing pilot programme in Ghana, Kenya and Malawi that has covered more than 800,000 children since 2019. The endorsement also tends to suggest that the vaccine had met the 50 per cent efficacy rate required for it to be made available to the public. In an earlier clinical trial of 15,000 patients conducted at 11 centres in seven African countries, carried out nearly 10 years ago, there was 46 per cent reduction in cases of malaria infection in children between the ages of five months and 17 months old who were vaccinated with RTS,S, while infants aged between six and 12 weeks had 27 per cent reduction.
The painstaking efforts and rigorous research works of scientists, scholars, WHO, donors and researchers that have made this break-through possible are commendable. According to the World Malaria Report 2020, of the 87 countries that were malaria endemic in 2019, 29 countries (mostly African countries) accounted for 95 per cent of malaria cases globally with Nigeria leading the pack at 27 per cent. It further states that 95 per cent of global malaria deaths were in 32 countries (mostly African) with Nigeria leading and accounting for 23 per cent of the deaths. Given the prevalence rate of malaria in Africa, the vaccine should be welcome as a beneficial medical scientific discovery.
However, Africa still has a long way to go in taking charge of its affairs. While it is convenient to accuse external ultra-capitalist influences as agents of disempowerment, African organisations have been found wanting in embarking on problem-solving initiatives. It could be recalled that nearly 10 years ago, GlaxoSmithKline refused to scheme Africa and other poorer nations into the clinical trials of this same vaccine until the Bill and Melinda Gates Foundation doled out $200 million through the nonprofit PATH Malaria Vaccine Initiative to include them in the trials. Such initiatives, as philanthropic as they seem, reiterate in an embarrassing manner Africa’s eternal dependence on Western donors to solve their problem. But for the intervention, African countries could have been eternally dependent on foreigners for remedy of a disease that is mostly Africa-bound.
Therefore, beyond the philanthropy of foreign donors, Africa as a people must learn to initiate moves to solve its own problems. It is embarrassing to African collective intellect that some powers are empowering their societies and enriching their economies by solving our problems.
Furthermore, Nigeria, the most malaria endemic country in the world, was not part of countries in which trials and pilot studies were carried out. What message does this signal to the Nigerian authorities and its people? It suggests Nigeria as a reliable consumer listing in the pharmaceutical capitalism and a beggarly appendage in the political economy of malaria.
The new malaria vaccine should invoke in Nigerians, frank and somber moments of actionable rethinking as a people. Now that the vaccine has been endorsed for public use, Nigerian scientists and consumer protection experts must go to work to ascertain the efficacy and long-term safety of this vaccine for children. They can do this through continuous and diligent scrutiny of the use of the vaccine even if trials and a prior pre-market approval had been carried out. Nigerians need to know the side effects of the vaccine, if any, on fertility, immunity, body organs and neurological function in the long term.
The Nigerian Academy of Science and its medical and engineering equivalents should institute massive knowledge production schemes that can solve African problems rather than being servile collaborators to initiatives that suppress African knowledge production systems. They should throw their weight behind local scientists who are painstakingly developing homegrown solutions to local health problems rather than unfairly prejudge and persecute the latter through some punitive scientific grandstanding. Indigenous scientists, medical and science academies should also be at the forefront to authenticate claims of traditional medicine practitioners who have made audacious efforts towards local remedies of malaria and others diseases.
Some Nigerian scientists have reportedly expressed frustration over regulatory bodies’ handling of their discoveries. Whilst these
claims are yet to be verified, it is instructive to inform Nigerian regulatory bodies such as the National Agency for Food Drug Administration and Control (NAFDAC) that this is not the time to assume the role of a pit-bull for foreign institutions. There is need for an independent, realistic and nationalistic NAFDAC – one that is not tied to the apron-strings of the superpowers.
At policy level, African and Nigerian medical and scientific research organisations should initiate home grown modalities to address medical problems rather than wait for special foreign organisations and research agencies of powerful western nations which impose unfavourable conditions to their offers, often turning locals into experimental guinea-pigs for their own medical research initiatives. A nationally guided pro-active research should be instituted.
Nature and providence have endowed this country with the resources it needs to address its environmentally generated medical problems, including malaria. Therefore, African researchers should reflect deeply and use today’s technology and scientific refinement to bridge the resourcefulness of their forebears and health challenges. What is needed to drive this is a self-redirection by the government and a re-orientation of people’s mentality.
 Follow Us on Google News
Follow Us on Google News
 Follow Us on Google Discover
Follow Us on Google Discover