The virus is old and cold and Africa is young and hot. — Anglophone slogan
In the continent, malaria is our problem.
In this period of coronavirus,
it’s surprising an antibody — Akhaine
The COVID-19 pandemic is on course, and vaccines are at various levels of clinical trials and dogged by an egoistic struggle about which country is first to roll out a vaccine. Kremlin says it is first in this global race to rein in the pandemic. Intriguingly, a naive government sitting Abuja, Nigeria’s capital territory has already ordered the Russian vaccine without mindful of the politics of the process. The US and its allies don’t trust the Slavonic stock.
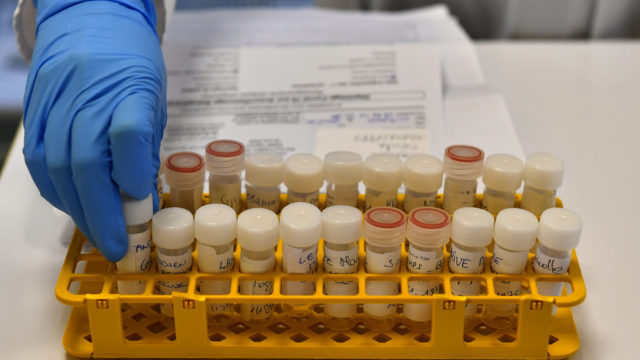
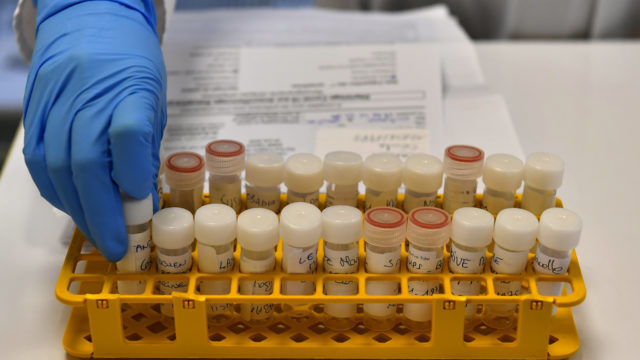
The politics of cure is not over with the presence of a powerful pharmaceutical complex. In managing COVID-19 the oral medication, hydroxychloroquine and remdesivir have been in the front burner with their controversial baggage. I undertake a brief review of these medications and speculate in the absence of controlled clinical trials that the delayed African winter of COVID-19 might be as a result of our use of chloroquine as both preventive and curative for the malarial scourge in Africa. Before now there has been a variety of explanations as to why the virus is yet to overwhelm the continent. In a personal communication with my American friend, Dave Peterson, he wondered why the virus seemed not to take its toll on Africa and went further to suggest that hot climatic conditions could be responsible for the low rate of infection. My rebuttal was we were not testing enough for any informed opinion on the scale of infection. Coming back to this subject, I find the analysis of Olivier Marbot in his article titled, “Coronavirus: Unpacking the theories behind Africa’s low infection rate” published in The Africa Report, May 2020 helpful in charting the arguments once again. Climate, youthful population, lower population density, less travel, experience with epidemics, effective cross-border cooperation, indirect protection from other treatments, ‘genetic’ immunity, viral mutation, and better masks. On climate, it is argued that COVID-19 thrives in the temperate weather than in a hot one, a theory that seemed to have been supported by the epidemiological map of COVID-19.
It is equally backed by the research information that respiratory diseases are less common in hot dry countries and that the virus’ half-life declines a great deal with increased temperature and humidity.
However, in vitro experiment with the coronavirus proves the contrary as the virus thrives without inhibition from heat. Youthful demographics features in the debate as the elderly are proven to more susceptible to COVID-19 than the young; and the continent with a youthful population in which median age is put at 19.4 years is spared. Africa has less densely populated cities and this reality seems to impact the spread of COVID-19. Africa is less travelled, it is argued. This buttressed by the fact that “on average, than the populations of most developed countries, and as a result infection risks are inevitably greatly reduced…In addition, just one African airport – that of Johannesburg – features in the list of the 50 busiest airports in the world”. A compelling point is a fact that the continent has lived and managed deadly diseases such as Ebola and that experience has been handy in managing COVID-19. In this regard, Ugandan President Yoweri Museveni’s address at the outbreak of COVID-19 is evident enough. Another compelling factor summoned is the fact of Africa’s personality or solidarity which has accounted for effective cross-border cooperation allowing for share facility and aiding of each other.
Yet another point is the indirect protection from other treatments. In Marbot’s words, “…there are less coronavirus infections in the countries most impacted by malaria or tuberculosis. The same holds true for countries that vaccinate much of their population with Bacillus Calmette-Guérin (BCG)”. And indeed, “many doctors think that antimalaria treatments like chloroquine have a certain amount of effectiveness. Given that a lot of people have been treated with these drugs in Africa, a resistance could be present”.
‘Genetic’ immunity is summoned in the argument but less supporting evidence. It could be a viral mutation with a benign variant circulating in the continent.
This is completed by better masks from our quality textile materials. Interesting! But Marbot’s supplies the verdict of the science community: the earliest and authoritarian approach to lockdown might have saved the day. The argument about the slow-motion of infection could be taking to the realm of medication which itself is dogged by controversy. Some have averred that Hydroxychloroquine cures COVID-19. Professor Harvey A. Risch of Yale University did a study on this species of medication and affirmed its utility.
Recently, the Texas-based Medical Doctor, Stella Emmanuel declared ex-cathedra its effectiveness taking along with other medications drawing on her experience as a general practitioner. Beyond these affirmations, it is common knowledge that Nigerian doctors have managed COVID-19 along with other immune-boosting medications. In the COVID-19 inferno, the US, even remdesivir has been administered to COVID-19 patients.
On hydroxychloroquine claim to value, I rely on Risch’s arguments in the July 23, 2020, Newsweek opinion and research journal here. Risch, a professor of epidemiology at Yale School of Public Health, with over 300 peer-reviewed publications to boot is confounded by the policticisation of a medication “that the data fully support but which, for reasons having nothing to do with a correct understanding of the science, has been pushed to the sidelines.
As a result, tens of thousands of patients with COVID-19 are dying unnecessarily”. He stressed the fact that hydroxychloroquine administered “ very early in the course of illness, before the virus has had time to multiply beyond control, it has shown to be highly effective, especially when given in combination with the antibiotics azithromycin or doxycycline and the nutritional supplement zinc”.
These points have well-argued with all the data in a major journal article titled, “Early Outpatient Treatment of Symptomatic, High-Risk COVID-19 Patients that Should be Ramped-Up Immediately as Key to the Pandemic Crisis” published in the American Journal of Epidemiology (AJE) on May 27, 2020. Risch salutes physicians who have resorted to the medications despite widespread uncertainty and passes them as heroes for following the path of science. To add, Risch is saddened by the politicisation of the medications and remarked that “When doctors graduate from medical school, they formally promise to make the health and life of the patient their first consideration, without biases of race, religion, nationality, social standing—or political affiliation. Lives must come first”. Interestingly, earlier on March 30, 2020, United States Federal Drugs Administration (USFDA) had given Emergency Use Authorisation (EUA) to chloroquine and hydroxychloroquine in the treatment of COVID-19, in the absence of approved indication.
Another pro-life argument comes about remdesivir, an all-purpose antiviral drug. Experts say remdesivir is the most promising repurposed candidate drug that has shown a consistent inhibitory effect both in vitro and in vivo against COVID-19 and members of the corona family such as SARS-CoV-1, MERS-CoV, and SARS-CoV-2. Indeed, Risch argued in his aforementioned journal paper that “Remdesivir has been studied extensively in laboratory work and in animals (8) and for other viral diseases and has good biological properties, suggesting utility for SARSCoV-2 infection”.
Awadhesh Kumar Singh, Akriti Singh, Ritu Singh, and Anoop Misrad in their article titled, “Remdesivir in COVID-19: A critical review of pharmacology, pre-clinical and clinical studies” published in Diabetes & Metabolic Syndrome: Clinical Research & Reviews, May 2020 offered a great insight into the utility of remdesivir to the extent that remdesivir accelerate recovery time and useful in severe cases of COVID-19, being the rationale for EUA for its use “only to treat adults and children with suspected or laboratory confirmed COVID-19…” The authors conclude that “Remdesivir appears to have optimal safety profile although its efficacy in the treatment of COVID-19 appears to have a mixed outcome at the moment”.
In a seeming introductory remark, Marbot notes that “Statistically speaking, Africa is an outlier…The continent, which is home to 17% of the world’s population, accounts for only 1.1% of cases and 0.7% of deaths. Even better news: with more than 12,000 recovered patients already, Africa appears to be more resistant to the coronavirus than other continents”. And now the percentage is 4.78 of the world’s cases and 3.52 of the global deaths from the virus.
Given the above facts about hydroxychloroquine and COVID-19, the debate about the low rate of infection in Africa and the corresponding low death rate can be contextualised. In fact, some folks in Ekpoma, a Midwestern town in Nigeria, argued in a conversation that COVID-19 lethality is mythical. Apart from potent herbal remedies, they argued that our routine consumption of chloroquine and sundry antimalarial medications both as prophylactic and curative has made us resistant to the worst fears of COVID-19. Africa seems to puzzle Bill and Melinda Gates and fellow modelers who are expecting a harvest of cadavers in the much-maligned continent. It is not yet time to let off our guard.
Akhaine is a Professor of Political Science, Lagos State University.
 Follow Us on Google News
Follow Us on Google News
 Follow Us on Google Discover
Follow Us on Google Discover