[dailymotion code=”k4HcJk4KaUjCB8wKXAu” autoplay=”yes”]
As humanity seeks herd immunity from coronavirus, the apprehension being expressed in many quarters over the safety of vaccination is significant. It signposts, on the one hand, that the vaccine candidates’ option against the dreaded virus is not yet of universal acceptability, and therefore, the search for a permanent and less controversial cure works in progress.
On the other hand, Nigeria and indeed the rest of the world cannot afford to ignore vaccination, given the absence of a more viable alternative cure now, and the potential collateral damages that may ensue from rejecting the vaccine.
In the midst of on-going global mass vaccination, therefore, caution remains a keyword, even as the authorities seek to debunk expressed fears on the jab. Clearly, a life-saving needle that defuses the killer virus is a welcome development and jab-seekers should have free access to vaccines. The general public is nonetheless entitled to make informed decisions on vaccination without being compelled.
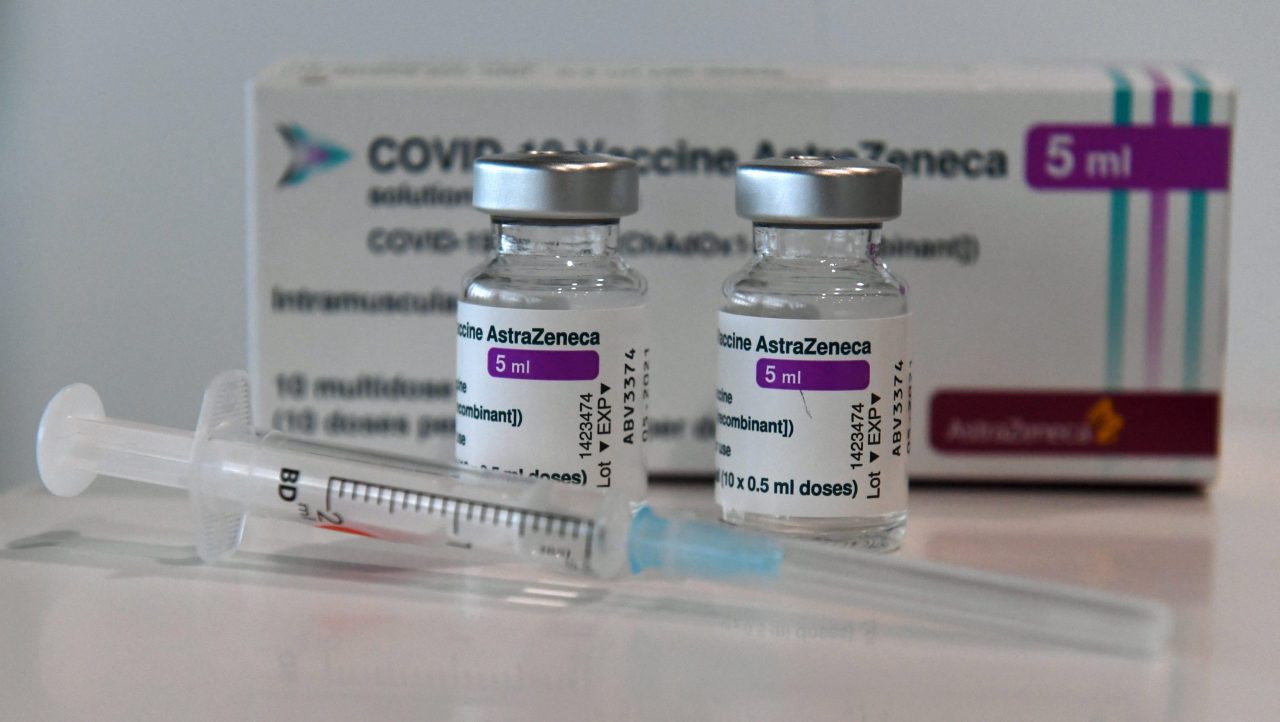
The Astra-Zeneca (AZ) vaccine, donated by the World Health Organisation’s Covax initiative, is making rounds across states of the federation, after President Muhammadu Buhari and state governors, except in Kogi, received jabs and urged Nigerians to follow suit as the country aims to inoculate 80 million people this year. But the process is already polarised between vaccine rush and vaccine hesitancy. At some centres are long queues of the general public-facing hiccups to get the COVID-19 vaccine. In other places are priority groups, among them health workers, who would not want to be needed so soon.
This hesitancy is not peculiar to Nigeria. Last week, about 16 European countries including Germany, France, Italy, and Spain, suspended the use of AZ vaccine following reports that a handful of people developed blood clotting adverse consequence after receiving it. Some regulators including the World Health Organisation (WHO) have countered, describing the side effects as too marginal to blight the efficacy of the vaccine brand. They add that the risk of not getting vaccines far-outweighs the side-effects and that in any event, the administration of the vaccine has not been linked directly with the development of blood clotting. Between the divide is the wary public, including Nigerians, seeking protection from COVID-19 afflictions without possible additional lifelong health burdens.
Coronavirus is especially susceptible to controversies and conspiracy theories given its dynamic nature, transient knowledge base, and uncertainties that continue to colour its demographic behaviour. Vaccines that erstwhile took a minimum of four years to prepare were finalised in about 12 months of the pandemic. Albeit a modern miracle, that feat is bound to fuel outstanding controversies, doubts, and even socio-political and economic rivalry among the superpowers.
Ab initio, vaccines have proved to be good for humanity, as reflected in their successful application to several health ailments; the discovery of COVID-19 inoculation is another victory for human will-power to practically surmount challenges. Vaccine is a product that stimulates a person’s immune system to produce immunity to a specific disease. Immunity is the protection from an infectious disease. But even a miracle has its limits. Vaccines, just like drugs, are bound to have some side-effects no matter how minimal. There are recipients that will have allergies. So, traditionally, it takes a while to know possible fallouts or get things right with vaccines and rollout in massive herd quantity. Besides animal studies, vaccines, before now, require at least two years of human trials. But COVID-19 vaccines were rushed, inevitably, into an emergency, even crisis situation, presenting a realistic reason for some stakeholders to doubt the basis of about 95 per cent efficacy rating, or whether they should be called ‘vaccine’ in the first place. For instance, the AZ brand was not tested in Africa, whose patchy data show that the virus has not been as aggressive as it is in countries where the vaccines originated. Fact is that studies on the vaccines and long-term adverse events are still being gathered from recipients – typical of an experimental trial run.
Although the current vaccine may not be the ultimate solution to the coronavirus, it, however, drastically lowers the risk of dying from the disease, which far outweighs any side-effect already known of the vaccine. Vaccines are not the only possible remedy to tackling COVID-19; still very relevant are the current preventive measures in the forms of physical distancing, wearing face masks, and regular handwashing among other hygiene practices that must be adhered to, even after being inoculated. There are orthodox and traditional prophylaxes to consider, boosting resistance to, and immunity from the virus’ grip.
However, available vaccines should not be kept idle in refrigerators; rather, caution and well-guided rollout by the local authorities should guide their administration. Monitoring of adverse events among the inoculated should be a priority, at least, to increase the knowledge-base and build more public confidence in the exercise despite the current complexity. No one should be forced to take the jab against his/her wish.
It is disappointing that Nigeria, with its huge natural potentials, has failed to mobilise research bodies to develop and procure home-grown solutions for COVID-19; or to lead Africa for a local solution since the pandemic erupted. The action of the country, along with the other 53 sovereign African nations, in queuing for vaccination crumbs and dole out from rich countries to save its people leaves much to be desired. Particularly, it renders Africans hapless, with little or no choice, in the middle of international trade politics and medical controversies. But it is never too late to think through local solutions. The race to a permanent solution and herd immunity may just be starting.
 Follow Us on Google News
Follow Us on Google News
 Follow Us on Google Discover
Follow Us on Google Discover