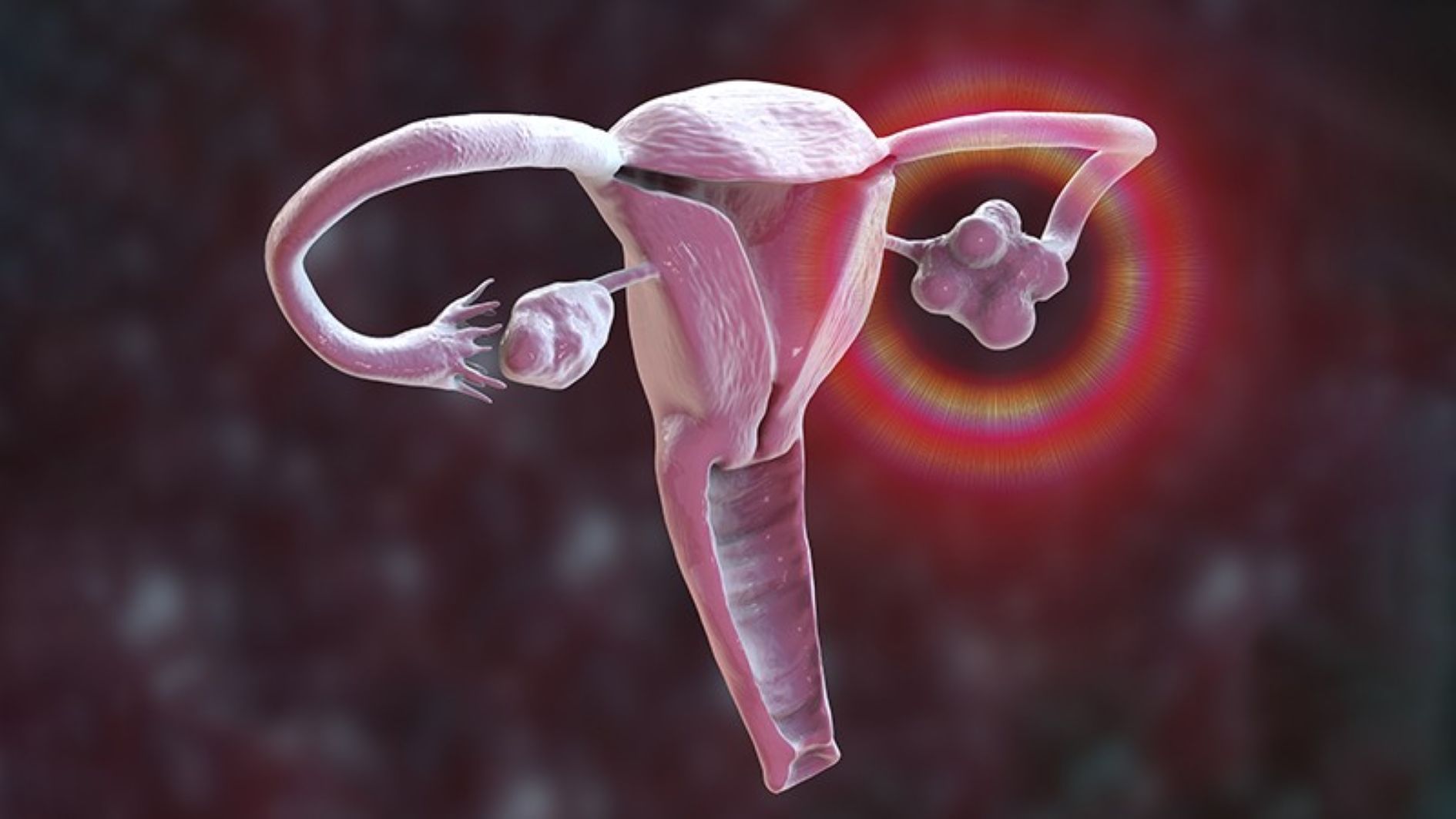
A major shift in women’s health care has emerged as polycystic ovarian syndrome (PCOS) has been officially renamed polyendocrine metabolic ovarian syndrome (PMOS) after 14 years of global advocacy, with experts describing the development as a landmark moment expected to improve diagnosis, treatment and long-term management of the condition.
The name change, formally announced in Prague and published in The Lancet, removes the longstanding emphasis on ovarian “cysts” and instead reflects the broader endocrine and metabolic nature of the condition, which experts say has long been misunderstood.
The condition was named nearly a century ago after surgeons operating on a woman observed sac-like structures on her ovaries alongside infertility and elevated male hormone levels. At the time, the structures were believed to be cysts, leading to the term “polycystic ovary syndrome.”
However, subsequent decades of research revealed that the condition extends far beyond reproductive health and affects multiple body systems, including metabolism, cardiovascular health and the skin. Earlier research has also linked the disorder to significantly higher risks of Type 2 diabetes.
Leading the global campaign for the renaming, Professor Helena Teede of Monash University said the so-called cysts were never true cysts but rather eggs whose development had been interrupted by broader endocrine disruption. According to her, the continued focus on ovaries and cysts contributed to misunderstanding of the condition and led to missed diagnoses and inadequate care for many women.
Under the latest diagnostic criteria, PMOS may be diagnosed when patients meet at least two of three conditions: elevated androgen levels, irregular menstrual cycles, and either high anti-mullerian hormone levels in blood tests or the presence of multiple arrested follicles seen on ultrasound imaging.
Teede explained that around 60 per cent of women can be diagnosed based on the first two criteria alone without requiring ovarian assessment, while others may use either blood testing or ultrasound examinations.
She added that blood testing may eventually reduce the need for internal ultrasounds because it is cheaper and more convenient for patients.
The coalition pushing for the change argued that the previous terminology created confusion among both patients and healthcare professionals and obscured the disorder’s metabolic and endocrine implications.
While noting that the new classification may improve research funding opportunities because studies on the condition would no longer be restricted mainly to ovarian or reproductive health funding streams; Teede acknowledged that resistance may emerge from businesses and influencers strongly associated with PCOS branding.
Despite affecting an estimated 170 million women of reproductive age globally and imposing major health and economic burdens, she said the disorder has historically received limited research investment.
According to The World Health Organization (WHO), the condition affects between 10 and 13 per cent of women of reproductive age globally, while up to 70 per cent of affected women remain undiagnosed.
The organisation also identifies the disorder as one of the leading causes of infertility worldwide and notes that women living with it face increased risks of obesity, insulin resistance, Type 2 diabetes and emotional health challenges.
Experts said international education and awareness campaigns targeting healthcare workers, governments and researchers will be rolled out during a three-year transition period before PMOS is fully adopted in the International Classification of Diseases in 2028.
 Follow Us on Google News
Follow Us on Google News
 Follow Us on Google Discover
Follow Us on Google Discover