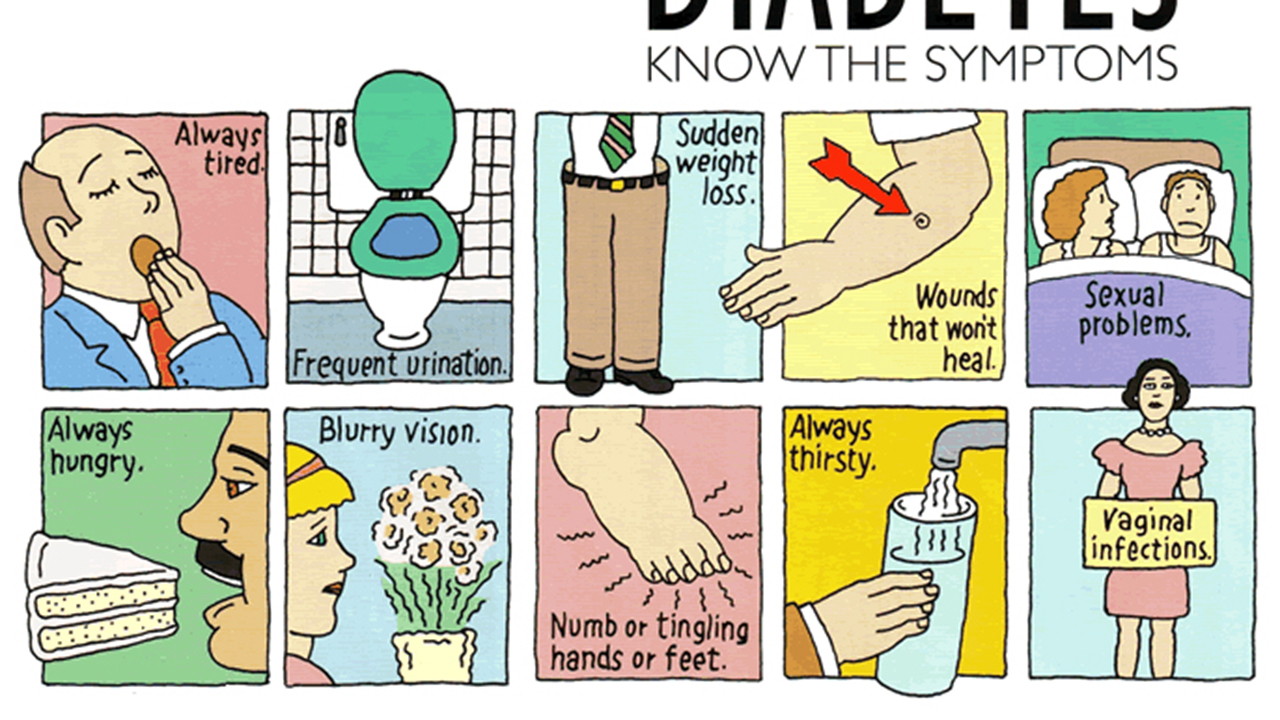
*Cutting out smoking, alcohol, eating well, exercising regularly decrease the chance of developing ailment by 75%
Researchers already know that excess body fat can increase the risk of diabetes, but a new study shows that one form of fat, in particular — the “invisible” one that accumulates around organs and intestines — can heighten this risk more than seven times, at least in women.
Though excess body fat is a known risk for many metabolic conditions, including type 2 diabetes, recent research has been gathering evidence to show that the amount of body fat is not the only factor that contributes to risk.
Now, research from Uppsala University in Sweden has found that the fat that accumulates around the organs and intestines — called visceral fat — is a crucial factor that raises the risk of type 2 diabetes, particularly in women.
The team — co-led by Torgny Karlsson, Ph.D. — studied the data of 325,153 individuals, which they accessed through the UK Biobank.
Visceral fat is “invisible,” and it can be difficult to find out how much a person’s body has stored. To do so, specialists must conduct expensive tests, such as MRI and CT scans or dual-energy X-ray absorptiometry.
Yet, in their study — the results of which appear in Nature Medicine — the researchers developed an easier, more cost-efficient method of estimating body fat that allowed them to then conduct further analyses, establishing how this form of fat contributed to health risks.
After calculating visceral fat estimates for their study cohort, the researchers conducted a genome-wide association analysis that allowed them to identify visceral fat as a top risk factor for hypertension, heart attack and angina, type 2 diabetes, and hyperlipidemia.
While the initial findings may come across as quite intuitive, the scientists faced a few unexpected results as well.
However, the researchers explain that this is not the case for all women. The risk increase, they say, occurs most rapidly in individuals who only have small or moderate amounts of visceral fat, to begin with.
Meanwhile, tall people may be protected against type 2 diabetes, research suggests. Each additional four inches (10cm) in height lowers the risk of developing the condition by 41 per cent for men and 33 per cent for women.
The researchers – from the German Institute of Human Nutrition Potsdam-Rehbruecke – believe this is because short people have higher liver fat content, blood pressure, and inflammation.
And tall people have greater insulin sensitivity and more efficient beta cells – a type of cell found in the pancreas, which makes insulin.
The researchers, who tracked 28,000 people, said height was a ‘useful predictive marker’ for diabetes risk.
Writing in the Diabetologia medical journal, they said: “Part of this inverse association may be driven by the associations of greater height with lower liver fat content and a more favourable profile of cardiometabolic risk factors, specifically blood fats, adiponectin, and C-reactive protein.”
They found that the association of height with diabetes risk appeared to be stronger among people with a normal weight, with an 86 per cent lower risk for men per every four inches of height, and 67 per cent lower risk for women.
In overweight or obese people each additional four inches was associated with a 36 per cent lower diabetes risk for men and 30 per cent lower risk for women.
They added: “This may indicate that a higher diabetes risk with larger waist circumference counteracts beneficial effects related to height, irrespective of whether larger waist circumference is due to growth or due to consuming too many calories.”
The authors also said that the increased risk in shorter individuals might be due to higher liver fat content and a “less favourable profile of cardiometabolic risk factors” – such as blood pressure.
They added: “Our findings suggest that short people might present with higher cardiometabolic risk factor levels and have higher diabetes risk compared with tall people.
“Our study also suggests that early interventions to reduce height-related metabolic risk throughout life likely need to focus on determinants of growth in sensitive periods during pregnancy, early childhood, puberty, and early adulthood, and should take potential sex differences into account.”
Meanwhile, people who lead the healthiest lifestyles maybe 75 per cent less likely to develop type 2 diabetes, research suggests.
Scientists at the Huazhong University of Science and Technology, China, analysed more than 1.1million people across 14 studies.
They discovered adults who ate well, exercised regularly and did not smoke were less likely to suffer from the killer condition.
And the team claims they found the risk goes down by up to 61 per cent with each ‘healthy habit’ a person adopted.
Diabetes aside, leading a healthy lifestyle also reduced the participants’ risk of dying from heart disease or cancer by up to 52 per cent.
The scientists hope their study shows that ‘lifestyle modification should be the cornerstone’ for diabetes prevention.
“Diabetes complications, particularly cardiovascular disease, are the leading cause of illness and death amongst individuals with type 2 diabetes,” the researchers wrote in the journal Diabetologia.
“Prevention of the condition and its long-term adverse outcomes is [therefore] urgently needed. We encourage people to adopt healthy living habits for example as regards diet, activity, smoking, and drinking.”
More than half a billion people worldwide are thought to have type 2 diabetes, with 22million new cases occurring every year.
With cases on the rise, the Chinese scientists set out to uncover how healthy habits could prevent the disease.
Fourteen existing studies on the subject were identified from the US, Asia, Europe, and Oceania.
Participants were monitored for at least three lifestyle habits, like diet, activity and alcohol consumption. They were followed for a minimum of a year.
Ten other studies were also included. These had 34,385 types 2 diabetics from across the world, followed for between four and 21 years.
The scientists weighted each of the studies based on their number of participants. Healthy habits were then tallied via a points system.
Overall, around 14 per cent of the participants stuck to the healthiest lifestyle, while 11 per cent opted for the least healthy option.
Those who exercised the most ate well and did not smoke, were 75 per cent less likely to develop type 2 diabetes than their least healthy counterparts.
Several of the studies suggested that for every ‘good’ habit a person adopts, their risk of the disease goes down by between 11 and 61 per cent.
Although obesity is linked to type 2 diabetes, body weight was found to be less of a factor in the condition’s onset than a combination of other lifestyle habits.
The researchers wrote that their findings support the recommendations from the American Diabetes Association and other organisations that lifestyle modification should be the cornerstone for the management of diabetes’.
“Healthy lifestyle interventions could reduce cardiovascular disease outcomes in persons with type 2 diabetes,” they added.
“Given that the proportion of individuals with the healthiest lifestyle was found to be low in most populations, promotion of an overall healthy lifestyle, instead of tackling one particular lifestyle factor, should be a public health priority for all countries.”
Future studies should investigate the link between lifestyle habits and type 2 diabetes in other ethnic groups, they added.
Most of the studies in their review were carried out in high-income countries, with white participants.
With type 2 diabetes rising in children and teenagers, studies should also look at how healthy habits could prevent the disease in these age groups.
[ad unit=2]
 Follow Us on Google News
Follow Us on Google News
 Follow Us on Google Discover
Follow Us on Google Discover
