• Long-term high-fat diet expands waistline, shrinks the brain, causes anxiety, depression, say, scientists
• Big burst of exercise at weekend as good as spreading activity out across week in lowering chances of death
• Daily avocados improve diet quality, help lower cholesterol levels, and heart attack risk, researchers find
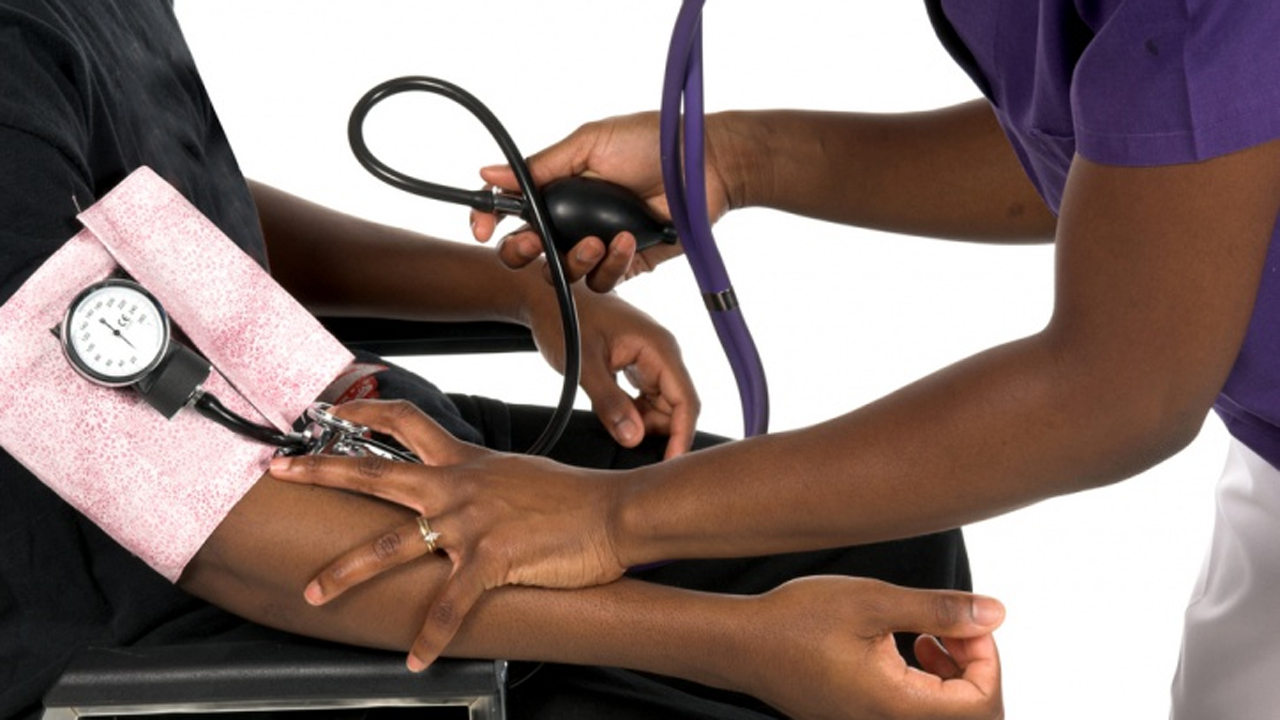
People who add extra salt to their food at the table are at higher risk of dying prematurely from any cause, according to a study of more than 500,000 people, published in the European Heart Journal on Monday.
Compared to those who never or rarely added salt, those who always added salt to their food had a 28 per cent increased risk of dying prematurely. In the general population, about three in every 100 people aged between 40 and 69 die prematurely. The increased risk from always adding salt to food seen in the current study suggests that one more person in every 100 may die prematurely in this age group.
In addition, the study found a lower life expectancy among people who always added salt compared to those who never, or rarely added salt. At the age of 50, 1.5 years and 2.28 years were knocked off the life expectancy of women and men, respectively, who always added salt to their food compared to those who never, or rarely, did.
The researchers, led by Professor Lu Qi, of Tulane University School of Public Health and Tropical Medicine, New Orleans, USA, say their findings have several public health implications.
“To my knowledge, our study is the first to assess the relationship between adding salt to foods and premature death. It provides novel evidence to support recommendations to modify eating behaviours for improving health. Even a modest reduction in sodium intake, by adding less or no salt to food at the table, is likely to result in substantial health benefits, especially when it is achieved in the general population,” said Prof. Lu Qi, of Tulane University School of Public Health and Tropical Medicine, New Orleans, United States of America (USA).
“Assessing overall sodium intake is notoriously difficult as many foods, particularly pre-prepared and processed foods, have high levels of salt added before they even reach the table. Studies assessing salt intake by means of urine tests often only take one urine test and so do not necessarily reflect usual behaviour. In addition, foods that are high in salt are often accompanied by foods rich in potassium, such as fruit and vegetables, which is good for us. Potassium is known to protect against the risk of heart diseases and metabolic diseases such as diabetes, whereas sodium increases the risk of conditions such as cancer, high blood pressure and stroke,” Qi said.
For these reasons, the researchers chose to look at whether or not people add salt to their foods at the table, independent of any salt added during cooking.
“Adding salt to foods at the table is a common eating behaviour that is directly related to an individual’s long-term preference for salty-tasting foods and habitual salt intake,” said Qi. “In the Western diet, adding salt at the table accounts for six-20 per cent of total salt intake and provides a unique way to evaluate the association between habitual sodium intake and the risk of death.”
The researchers analysed data from 501,379 people taking part in the United Kingdom (UK) Biobank study. When joining the study between 2006 and 2010, the participants were asked, via a touch-screen questionnaire, whether they added salt to their foods (i) never/rarely, (ii) sometimes, (iii) usually, (iv) always, or (v) prefer not to answer. Those who preferred not to answer were not included in the analysis.
The researchers adjusted their analyses to take into account factors that could affect outcomes, such as age, sex, race, deprivation, body mass index (BMI), smoking, alcohol intake, physical activity, diet and medical conditions such as diabetes, cancer and heart and blood vessel diseases. They followed the participants for a median (average) of nine years. Premature death was defined as death before the age of 75 years.
“As well as finding that always adding salt to foods was linked to a higher risk of premature death from all causes and a reduction in life expectancy, the researchers found that these risks tended to be reduced slightly in people who consumed the highest amounts of fruit and vegetables, although these results were not statistically significant.
“We were not surprised by this finding as fruits and vegetables are major sources of potassium, which has protective effects and is associated with a lower risk of premature death,” said Qi.
He added: “Because our study is the first to report a relation between adding salt to foods and mortality, further studies are needed to validate the findings before making recommendations.”
In an editorial to accompany the paper, Professor Annika Rosengren, a senior researcher and professor of medicine at the Sahlgrenska Academy, University of Gothenburg, Sweden, who was not involved with the research, writes that the net effect of a drastic reduction in salt intake for individuals remains controversial.
“Given the various indications that a very low intake of sodium may not be beneficial, or even harmful, it is important to distinguish between recommendations on an individual basis and actions on a population level,” she writes.
She concludes: “Classic epidemiology argues that a greater net benefit is achieved by the population-wide approach (achieving a small effect in many people) than from targeting high-risk individuals (a large effect but only achieved in a small number of people).
The obvious and evidence-based strategy with respect to preventing cardiovascular disease in individuals is early detection and treatment of hypertension, including lifestyle modifications, while salt-reduction strategies at the societal level will lower population mean blood pressure levels, resulting in fewer people developing hypertension, needing treatment, and becoming sick. Not adding extra salt to food is unlikely to be harmful and could contribute to strategies to lower population blood pressure levels.”
The strength of Prof. Qi’s study is the large number of people included. It also has some limitations, which include: the possibility that adding salt to food is an indication of an unhealthy lifestyle and lowers socioeconomic status, although analyses attempted to adjust for this; there was no information on the quantity of salt added; adding salt may be related to total energy intake and intertwined with the intake of other foods; participation in UK Biobank is voluntary and therefore the results are not representative of the general population, so further studies are needed to confirm the findings in other populations.
Prof. Qi and his colleagues will be carrying out further studies on the relationship between adding salt to foods and various chronic diseases such as cardiovascular disease and diabetes. They also expect potential clinical trials to test the effects of a reduction in adding salt on health outcomes.
Meanwhile, new research shows that fatty foods may not only be adding to your waistline but also playing havoc with the brain.
An international study led by UniSA neuroscientists Professor Xin-Fu Zhou and Associate Professor Larisa Bobrovskaya has established a clear link between mice fed a high-fat diet for 30 weeks, resulting in diabetes, and a subsequent deterioration in their cognitive abilities, including developing anxiety, depression and worsening Alzheimer’s disease.
Mice with impaired cognitive function were also more likely to gain excessive weight due to poor metabolism caused by brain changes.
Researchers from Australia and China have published their findings in Metabolic Brain Disease.
UniSA neuroscientist and biochemist Associate Professor Larisa Bobrovskaya says the research adds to the growing body of evidence linking chronic obesity and diabetes with Alzheimer’s disease, predicted to reach 100 million cases by 2050.
“Obesity and diabetes impair the central nervous system, exacerbating psychiatric disorders and cognitive decline. We demonstrated this in our study with mice,” Associate Professor Bobrovskaya says.
In the study, mice were randomly allocated to a standard diet or a high-fat diet for 30 weeks, starting at eight weeks of age. Food intake, body weight and glucose levels were monitored at different intervals, along with glucose and insulin tolerance tests and cognitive dysfunction.
The mice on the high-fat diet gained a lot of weight, developed insulin resistance and started behaving abnormally compared to those fed a standard diet.
Genetically modified Alzheimer’s disease mice showed a significant deterioration of cognition and pathological changes in the brain while fed the high-fat diet.
“Obese individuals have about a 55 per cent increased risk of developing depression, and diabetes will double that risk,” Bobrovskaya says.
“Our findings underline the importance of addressing the global obesity epidemic. A combination of obesity, age and diabetes are very likely to lead to a decline in cognitive abilities, Alzheimer’s disease and other mental health disorders.”
Also, according to a study, a big burst of exercise at the weekend is as good as spreading activity out across the week.
United States (U.S.) researchers tracked 350,000 people over 10 years to see how well so-called weekend warriors fared.
The findings, in the JAMA Internal Medicine journal, suggest the type and total amount of exercise count, rather than how many sessions.
At least 150 minutes a week of moderate-intensity exercise is recommended.
Going for a brisk walk, a light effort cycle on a bike or playing doubles in tennis would count towards this.
Or you could do 75 minutes of vigorous activity – something like running, swimming or playing a game of football – say health experts in guidance published by the British National Health Service (NHS).
Many of the participants in the US study clocked up this amount in a week. But some crammed it into one or two sessions rather than spacing it out.
Those who reached their recommended level of activity, whether during the week or the weekend, had lower death risk than those who did less than the recommended amount.
The NHS also says people should do some form of physical activity every day including strength exercises and try not to stay seated for extended periods of time.
Strength exercises include yoga, pilates and heavy gardening.
Very vigorous activity that can help achieve recommended physical activity levels and can be done in shorter, sharper bursts, includes high-intensity interval training, spinning classes, lifting heavy weights and hill sprinting.
British Heart Foundation senior cardiac nurse Joanne Whitmore said: “This large study suggests that, when it comes to exercise, it doesn’t matter when you do it.
“The most important thing is that physical activity is undertaken in the first place.
“Whether you cram your exercise in on the weekend or spread it across the week, aim for 150 minutes of moderate-intensity activity each week.
“Exercise can improve your health, reducing your risk of heart and circulatory diseases like heart attack and stroke.
“Moderate-intensity activities make you breathe harder and make your heart beat faster than usual but you should still be able to have a conversation whilst doing them.”
Meanwhile, according to a new study, eating one avocado a day for six months was found to have no effect on belly fat, liver fat or waist circumference in people with overweight or obesity. However, it did lead to a slight decrease in unhealthy cholesterol levels.
In the randomised trial, the team — including Penn State researchers — also found that participants who ate avocados had better quality diets during the study period.
While prior, smaller studies have found a link between eating avocados and lower body weight, Body Mass Index (BMI), and waist circumferences, this was the largest, most extensive study to date on the health effects of avocados, including a large number of participants and length of the study period.
“While the avocados did not affect belly fat or weight gain, the study still provides evidence that avocados can be a beneficial addition to a well-balanced diet,” said Penny Kris-Etherton, Evan Pugh University Professor of Nutritional Sciences at Penn State. “Incorporating an avocado per day in this study did not cause weight gain and also caused a slight decrease in LDL cholesterol, which are all important findings for better health.”
Kristina Petersen, assistant professor of nutritional sciences at Texas Tech University, said the study also found that eating avocados daily improved the overall quality of the participants’ diets by eight points on a 100-point scale.
“Adherence to the Dietary Guidelines for Americans is generally poor in the U.S., and our findings suggest that eating an avocado per day can substantially increase overall diet quality,” Petersen said. “This is important because we know a higher diet quality is associated with lower risk of several diseases including heart disease, type 2 diabetes and some cancers.”
The research — recently published in the Journal of the American Heart Association — was conducted in conjunction with Loma Linda University, Tufts University, and UCLA, with coordinating support from Wake Forest University.
For the study, the researchers conducted a six-month experiment involving more than 1,000 participants experiencing overweight or obesity, half of whom were instructed to eat an avocado every day while the other half continued their usual diet and were told to limit their avocado consumption to less than two a month. Fat in the abdomen and around other organs was measured precisely using MRI before and at the end of the study.
“While one avocado a day did not lead to clinically significant improvements in abdominal fat and other cardiometabolic risk factors, consuming one avocado a day did not result in body weight gain,” said Joan Sabaté, professor at Loma Linda University School of Public Health. “This is positive because eating extra calories from avocados doesn’t impact body weight or abdominal fat, and it slightly decreases total and LDL-cholesterol.”
They also found that daily avocados resulted in total cholesterol decreasing 2.9 milligrams per deciliter (mg/dL) and LDL cholesterol decreasing 2.5 mg/dL.
The researchers said that in the future, they would continue to analyse data from the study. For example, participants were not instructed on how to eat their avocados each day, and future research could investigate how participants incorporated the avocados into their diet and whether any differences in the results are observed based on how participants ate the avocado.
 Follow Us on Google News
Follow Us on Google News
 Follow Us on Google Discover
Follow Us on Google Discover
