
It’s that time of year again when the global community recognises the need to commit to eliminate an ancient disease that dates back 4,000 years called ‘malaria’. It’s no secret that Nigeria, among the 87 endemic countries, has the largest proportion of malaria cases and deaths, especially in children under five.
[ad]
According to the 2022 WHO report, Nigeria had the highest number of malaria cases globally, accounting for approximately 27 per cent of all cases worldwide.
Nigeria also had the highest number of global malaria deaths, accounting for approximately 31 per cent of all malaria deaths worldwide in 2022.
Additionally, the country loses an estimated $1.1 billion (N645.7 billion equivalent) each year due to malaria-related absenteeism and treatment costs. However, it’s worth noting that malaria incidence and prevalence have fluctuated in Nigeria over the past ten years.
The recent malaria indicator survey (year) showed that there has been a gradual reduction in prevalence, the percentage of under 5 who have malaria, from 27 per cent in 2015 to 22 per cent in 2021.
One could attribute the reduction and progress in the decline of malaria cases and deaths to the natural decline resulting from urbanisation – malaria is largely a rural disease, and with the measure of urbanisation in Nigeria. Or you can use the measure of internal migration to urban areas, where there comes a natural decline in the number of cases seen. However, studies have shown that deliberate and consistent efforts to control and eliminate malaria in Nigeria have contributed to the progress we have recorded.
The National programme, with its different partners, including but not limited to Global Fund, the World Bank, U.S. President’s Malaria Initiative (PMI), Bill and Melinda Gates Funding, Islamic Development Bank, and UK Department for International Development (DFID), has supported interventions and programmes to increase access to malaria prevention and control measures, especially mosquito nets, improve malaria diagnosis and treatment at hospitals and within communities, distribute antimalarial drugs to a particular populations (under-5 children) in high-transmission areas to reduce the malaria parasite reservoir, work with communities to raise awareness about malaria prevention and control, and invest in new tools and technologies.
However, are these efforts enough to eliminate malaria in Nigeria? With the growing population, should there be considerations to increase the resources spent on preventing and treating malaria?
Before addressing these burning questions, let’s take a cue from other countries and learn from their successes. Out of the 40 countries that WHO has certified Malaria-free, only five of them are African countries.
More recently, in 2019, Algeria was certified Malaria-free and had achieved its goal of eliminating Malaria.
How did Algeria achieve this seemingly impossible task? In Algeria, much of the success has been attributed to universal health care coverage that ensured rapid malaria diagnosis and treatment, strong levels of political commitments (measure of investment into healthcare or malaria), including long-standing financial support from the national government, while implementing the standard WHO recommended interventions; robust integrated surveillance systems, effective vector control measures such as insecticide-treated bed net distribution and indoor residual spraying, which helped to reduce the mosquito population and prevent the spread of malaria and rapid response to outbreaks of the disease.
The country has made significant efforts to strengthen its healthcare systems, ensuring that accessible and free healthcare services are provided by a well-trained health workforce to all individuals, including migrants.
This commitment plays a crucial role in promptly identifying and treating malaria cases. Additionally, the country had strong national-level political commitment and ardently devoted resources, including financial support for the malaria program through domestic financing. Understanding the key driver of transmission was also a definitive step in the progress towards elimination which was the porous and expansive borders., Algeria tracked imported cases and implemented fit-for-purpose interventions using an integrated surveillance system. Looking beyond Africa, Malaria-free countries like Uzbekistan, Paraguay, and Argentina have achieved success through different approaches.

Uzbekistan received consistent support from the Global Fund through a result-based approach, Paraguay utilised community health workers to treat and eliminate malaria, and Argentina fostered cross-border collaborations.
Bringing these lessons learned home-Nigeria, in terms of domestic funding for malaria, is limited.
In Nigeria, in 2017, the government contributed 8 per cent of the total expenditure on malaria while 86 per cent came from households largely out of pocket. However, there is hope. Nigeria has shown a level of political commitment by inaugurating the End Malaria Council in 2022.
This is a public-private alliance dedicated to advancing the fight against this deadly disease. One of the council’s most important duties is to gather financial and service commitments to help bridge the funding gap for the National Malaria Strategic Plan and other malaria elimination efforts.
To support these commitments, the End Malaria Fund has been established to supplement and stretch Nigeria’s limited resources. In other countries where this council has been set up, more than $23 million has been invested into their national malaria programmes.
Universal Healthcare, which is key for the elimination of malaria in Nigeria, is hindered by several factors, including a weak primary healthcare system due to dilapidated health structures, shortage of healthcare workers, and poor referral systems, popularly known as the “japa syndrome”.
However, by tackling malaria, Nigeria can kill two birds with one stone: strengthen healthcare systems and save lives from malaria, as Algeria has successfully demonstrated.
Without strong and integrated healthcare systems, Malaria elimination in Nigeria will remain just (merely) a dream.
In addition to what has been mentioned, there are several other opportunities in Nigeria that can be taken advantage of to eliminate malaria. This includes, exploring the contribution of the private sector, increasing resources for other interventions and innovations, community mobilisation to reinforce testing and treatment, and applying a multi-ministerial approach to elimination.
Nigeria has a vibrant private sector, including private philanthropy, civil society organisation, formal and informal private sectors, which could be mobilised to contribute financially to the malaria elimination programme and support better case management at the community level.
The private informal sector, which includes Patent and Proprietary Medicine Vendors (PPMVs) and Community Pharmacists collectively also known as drugstore or chemist, could contribute significantly to the fight against malaria at the community level.
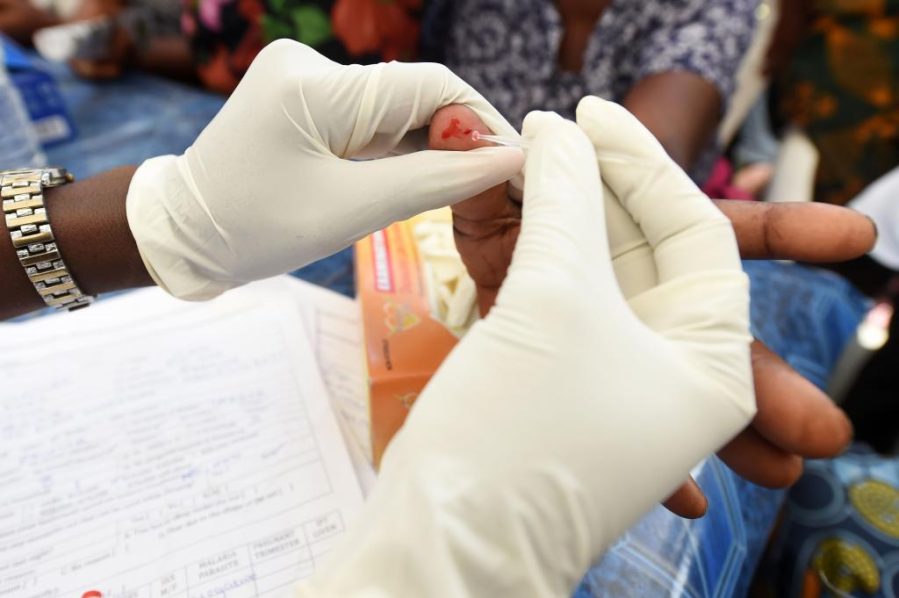
The 2021 malaria survey shows that over 56 per cent of fever cases visit the private informal sector for treatment. This means that most people at the community level will visit a drug store first when they have a fever.
There is an opportunity here to ensure that individuals visiting these drug stores receive appropriate testing and treatment.
Although the policy environment has been set to ensure that drug store owners can conduct simple rapid tests and treat with Artemisinin-based combination therapy.-ACT, testing at these stores remains remarkably low due to behavioural attitudes towards testing also known as “I know na malaria dey worry me, I no need testing”, wrong malaria messaging/advertising, limited availability of malaria commodities, and limited coordination of drug stores to ensure that all suspected fever cases are treated. Additionally, the country has strong community structures, activities, and programs that can be strengthened and leveraged to drive early identification, testing of suspected cases, and treatment of confirmed malaria cases. However, many of these community activities and systems need to be formalised, and capacity and resourcing strengthened.
Nigeria could also explore other interventions and innovations; the World Health Organisation has recommended two key interventions to control the malaria vector, including the use of nets and indoor residual spraying.
Nigeria and its development partners have invested heavily in the procurement and distribution of insecticide-treated nets, but the proportion of those who use the nets remains low.
This poor use is driven by several factors, including personal convenience- people reporting that they do not use their nets regularly due to the increasingly hot temperature in the country.
Therefore, there is a need to explore complementary interventions to control the malaria vector, such as indoor residual spraying (a method where special insecticide, not the regular “fleet or insecticide” is sprayed inside houses-on the walls to kill mosquitoes). Although this is considered capital intensive, indoor residual spraying does not require efforts from households, reducing the issues that come with net use, and has been a large contributing factor to elimination in some countries.
In terms of innovation, the recent malaria vaccine, the R21 Malaria Vaccine (Recombinant, Adjuvanted), is a welcoming development. Nigeria, through NAFDAC, has taken a great step by approving the vaccine. This is an opportunity to address malaria cases and deaths in the population most vulnerable to malaria mortality (under-5).
Lastly, there is a huge and imperative need to change the one-ministry approach to eliminating malaria and apply a multi-ministries approach. Different factors drive malaria transmission, such as environmental and behavioural factors, which require different ministries to work together.
An integrated approach will mean different ministries, such as Environment and Education, working with the Health Ministry to address factors that drive the infection beyond the health sector.
In conclusion, to answer the question “Can Nigeria completely eliminate malaria?” Yes, it’s possible to achieve elimination if we tackle the underlying issues, such as healthcare system challenges, and limited domestic funding for malaria and seize these available opportunities and innovations. Without putting in the work and remaining in status quo, malaria elimination remains a mere dream and aspiration.
Nigeria holds immense potential to eliminate malaria, but we haven’t reached that milestone yet.
[ad unit=2]
[ad unit=2]








