Practice reduces incidence of aggressive breast cancer, arsenic exposure in infants, influence immune system development in early life
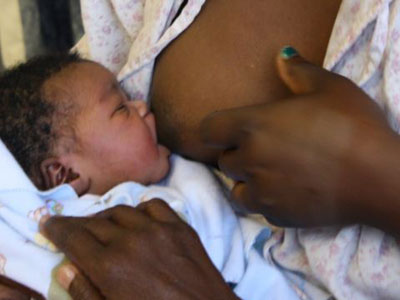
MORE reasons are emerging why Nigerian women must not only breastfeed their babies but exclusively for the first six months of life and continued with complementary feeding to about two years.
Reasons: Breastfeeding could significantly reduce infants’ risk of arsenic exposure; babies who were breastfed at one and six months had specific gut microbiome compositions, which may affect immune system development.
Also, baby’s diet during the first few months of life has a profound influence on the composition, diversity, and stability of the gut microbiome, which influence the baby’s ability to transition from milk to solid foods and may have long-term health effects; and low rates of breastfeeding in African American women may contribute to their higher incidence of the more aggressive and difficult-to-treat subtypes of breast cancer.
New findings published in the Journal of the National Cancer Institute suggest that low rates of breastfeeding in African American women may contribute to their higher incidence of the more aggressive and difficult-to-treat subtypes of breast cancer.
Women who have had children (parous women) appear to have an increased risk of developing estrogen receptor-negative breast cancer, the subtype that carries a higher mortality rate and is more common in women of African ancestry. A similar relationship was found for triple-negative breast cancer.
However, the association between childbearing and increased risk of estrogen receptor-negative and triple-negative breast cancer was largely confined to the women who had never breastfed.
Researchers from Boston University’s Slone Epidemiology Center (SEC) collaborated with the Roswell Park Cancer Institute of Buffalo, New York and the University of North Carolina Lineberger Cancer Center to form a consortium to study the determinants of breast cancer subtypes in African American women. They combined data on breast cancer cases and controls from four large studies, including the Boston University Black Women’s Health Study. The combined analyses included 3,698 African American women with breast cancer, including 1,252 with the estrogen receptor-negative subtype.
They found that parous women had a 33 percent higher chance of developing estrogen receptor negative breast cancer than women who had never given birth. Women who had four or more births and had never breastfed any of their babies had a 68 percent higher chance of developing this type of cancer compared with women who had only one birth and had breastfed that baby. By contrast, parous women who had four or more births had a slightly decreased risk of estrogen receptor-positive breast cancer, regardless of whether or not they had breastfed.
Also, another new study published in the journal Environmental Health Perspectives found that arsenic concentrations in the urine of breastfed infants were 7.5 times lower than those of infants who were formula fed.
Conducted by researchers from Dartmouth College in Hanover, New Hampshire, United States, the study found that infants who were breastfed had much lower levels of arsenic in their urine, compared with infants who were formula fed.
Lead author Prof. Kathryn Cottingham, of the Children’s Environmental Health and Diseases Prevention Research Center at Dartmouth said: “This study’s results highlight that breastfeeding can reduce arsenic exposure even at the relatively low levels of arsenic typically experienced in the United States. This is an important public health benefit of breastfeeding.”
Arsenic is a naturally occurring element found in water, rocks, soil and air, as well as in plants and animals. The most common sources of arsenic in humans is food, including some rice and dairy products, and water – particularly water that comes from ground sources, such as wells.
Exposure to arsenic at high levels has been associated with cancer, gastrointestinal disorders and other diseases. Early-life exposure to arsenic has been linked to fetal death, reduced birth weight and impaired cognitive functioning.
The authors note, however, that drinking water from private wells is also a primary source of arsenic exposure, and that families with these wells should get their tap water tested for arsenic.
Meanwhile, a series of studies set to be presented at the American Academy of Allergy, Asthma & Immunology’s Annual Meeting in Houston, TX, claim an infant’s immune system development and susceptibility to asthma and allergies may be influenced by a number of factors that shape what bacteria is in their gut, such as gestational age at birth, breastfeeding and delivery by Cesarean section.
Babies who were breastfed at one and six months had specific gut microbiome compositions, which the researchers say may affect immune system development.
The research team, including Dr. Christine Cole Johnson, chair of the Department of Public Health Sciences at Henry Ford Hospital in Detroit, Michigan, United States, said: “The findings further support the hygiene hypothesis – the idea that early childhood exposure to pathogens affects later-life risk of disease.
“For years now, we’ve always thought that a sterile environment was not good for babies. Our research shows why. Exposure to these micro-organisms, or bacteria, in the first few months after birth actually help stimulate the immune system.
“The immune system is designed to be exposed to bacteria on a grand scale,” she adds. “If you minimize those exposures, the immune system won’t develop optimally.”
 Follow Us on Google News
Follow Us on Google News
 Follow Us on Google Discover
Follow Us on Google Discover
